Review Article Open Access
The Role of Overtube-assisted Deep Enteroscopy ERCP in Roux-en-Y Gastric Bypass Patients
| Mohammad F. Ali*, Haseeb Ahmed and ShahzadIqbal | |
| Winthrop University Hospital, Department of Gastroenterology, Hepatology and Nutrition,Mineola, NY, USA | |
| Corresponding Author : | Mohammad F. Ali, MD Winthrop University Hospital Department of Gastroenterology Hepatology and Nutrition, Mineola, NY, USA E-mail: mfali@winthrop.org |
| Received August 22, 2014; Accepted September 20, 2014; Published September 25, 2014 | |
| Citation: Ali MF, Ahmed H, Iqbal S (2014) The Role of Overtube-assisted Deep Enteroscopy ERCP in Roux-en-Y Gastric Bypass Patients. J Obes Weight Loss Ther 4:229. doi:10.4172/2165-7904.1000229 | |
| Copyright: © 2014 AliMF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Bariatric surgery is the fastest growing medical intervention for obesity performed in theUS and Roux-en-Y Gastric Bypass (RYGB), is considered the "gold standard"comprising more than 60% of these cases. However, patients with surgically alteredanatomy after undergoing RYGB pose serious challenges to the endoscopist whenaccess to the biliary or pancreatic systems is required. Hurdles include reaching themajor papilla after navigating the length of the roux limb (often >100 cm) given thelimitations of standard gastroscopes and even push enteroscopes in achievingsufficient depth of insertion, orientation (upside-down configuration of the papilla), andthe lack of accessories that are actually designed for the long endoscopes required forperforming ERCPs in this patient population. To work around the aforementioned problems—specifically the length of the Rouxlimb— innovative techniques, notably overtube systems have been developed to allowthe enteroscope to reach the ampulla and perform ERCP. Three overtube-systems arepresently available: Double-balloon Enteroscopy (DBE), Single-balloon Enteroscopy(SBE), and Spiral Enteroscopy (SE). This review is designed to describe the role of these 3overtube systems in assisting with ERCP in RYGB patients based on existing literatureand evaluate their success rates in reaching the ampulla, diagnostic & therapeuticyields, and complication rates. Our review shows good success rates when comparing ability to reach ampulla (DBEERCP:83%; SBE-ERCP: 71%; SE-ERCP: 70%), diagnostic (DBE-ERCP: 77%; SBEERCP:55%; SE-ERCP: 41%) and therapeutic yields (DBE-ERCP: 75%; SBE-ERCP:81%; SE-ERCP: 68%) with low complication rates for all three systems. The sheer volume of RYGB procedures being performed and the associated predictedincrease in complications will lead to advanced endoscopists encountering morepatients with surgically altered anatomy and our review provides evidence thatovertube-assisted systems are effective and safe, and should be considered as a firstline modality in RYGB patients requiring ERCP.
To work around the aforementioned problems—specifically the length of the Rouxlimb— innovative techniques, notably overtube systems have been developed to allowthe enteroscope to reach the ampulla and perform ERCP. Three overtube-systems arepresently available: Double-balloon Enteroscopy (DBE), Single-balloon Enteroscopy(SBE), and Spiral Enteroscopy (SE). This review is designed to describe the role of these 3overtube systems in assisting with ERCP in RYGB patients based on existing literatureand evaluate their success rates in reaching the ampulla, diagnostic & therapeuticyields, and complication rates.
Our review shows good success rates when comparing ability to reach ampulla (DBEERCP:83%; SBE-ERCP: 71%; SE-ERCP: 70%), diagnostic (DBE-ERCP: 77%; SBEERCP:55%; SE-ERCP: 41%) and therapeutic yields (DBE-ERCP: 75%; SBE-ERCP:81%; SE-ERCP: 68%) with low complication rates for all three systems.
The sheer volume of RYGB procedures being performed and the associated predictedincrease in complications will lead to advanced endoscopists encountering morepatients with surgically altered anatomy and our review provides evidence thatovertube-assisted systems are effective and safe, and should be considered as a firstline modality in RYGB patients requiring ERCP.
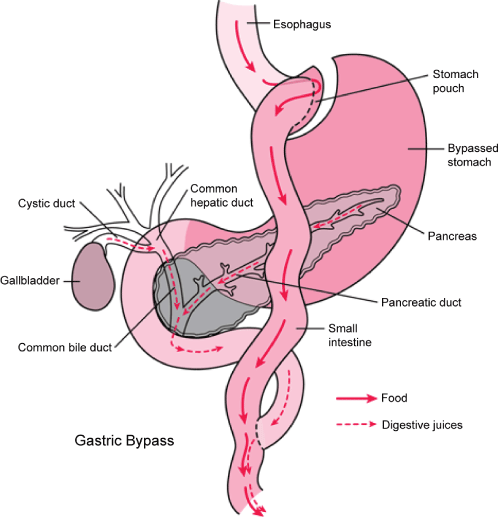
RYGB entails creating a small gastric pouch (<30ml) that is divided and separated from the distal stomach and anastamosed to a Roux limb of small bowel 75 to 150 cm in length [9,10]. The small gastric pouch and the narrow anastamotic outlet restrict caloric intake, while the major digestion and absorption of nutrients follow in the common channel (Figure 1) where gastric acid, pepsin, Intrinsic Factor (IF), pancreatic enzymes, and bile mix with ingested food [11].
Patients with surgically altered anatomy after undergoing RYGB pose serious challenges to the endoscopist when access to the biliary or pancreatic systems is required. The first hurdle is reaching the major papilla after navigating the length of theroux limb (often >100 cm). Studies have shown the limitation(s) of standard gastroscopes and even push enteroscopes in achieving sufficient depth of insertion in these patients [12,13]. The second hurdle/obstacle involves the orientation. Endoscopists use front viewing scopes so they are not habituated to the upside-down configuration of the papilla in RYGB patients, making cannulation difficult [14]. The third barrier is the lack of accessories that are actually designed for the long endoscopes required for performing Endoscopic Retrograde Cholangiopancreatographies (ERCPs) in this patient population [14,15]. Table 1 lists available enteroscopy length ERCP accessories.
To work around the aforementioned problems—specifically the length of the Roux limb— innovative techniques notably overtube systems have been developed to allow the enteroscope to reach the ampulla and perform ERCP. Three overtube-systems are presently available: Double-balloon Enteroscopy (DBE), Single-balloon Enteroscopy (SBE), and Spiral Enteroscopy (SE). This review is designed to describe the role of these 3 overtube systems in assisting with ERCP in RYGB patients based on existing literature and evaluate their success rates in reaching the ampulla, diagnostic & therapeutic yields as defined below, and complication rates.
Therapeutic yield has been defined as the ability to successfully carry out an endoscopic therapy when indicated in patients who have been successfully cannulated.
In one of the first case series by Emmett DS and Mallat DB describing DBE-ERCP in 6 patients with Roux-en-Y gastric bypass surgery, the ampulla was successfully reached in 100% of the cases, with adequate cannulation of either the biliary or pancreatic duct in 88% of these [19]. Therapeutic interventions ranged from stone removal to pancreaticobiliary-duct dilation to sphincterotomy. The mean total duration of the procedure was 99+/-48 minutes and there was no reported immediate or short-term complications.
Given the forward-viewing nature of the endoscopes used for ERCP and the limited number of accessories compatible with the standard double enteroscope due to its length, cannulation of the native papilla may be difficult with DBE-ERCP. This issue can be overcome with the use of a ‘short’ DBE system that has a 152 cm working length and is compatible with conventional accessories.
A multicenter study by Siddiqui et al. performed ERCPs in 39 RYGB patients using the ‘short’ double balloon enteroscope (EC-450BI5; Fujinon), achieving successful bile duct cannulation in 29 of the 32 patients in whom the papilla/surgical anastomoses was reached. A full spectrum of therapeutic maneuvers were performed, including sphincterotomy, stone extraction, balloon dilation, and the insertion of plastic/metal stents [20-25]. Additionally, studies have been done by Moreels et al. [22] and Patel et al. [26] demonstrating the feasibility of diagnostic and therapeutic DBE-ERCP in large cohorts of patients who had undergone a variety of of Roux-en-Y reconstructive surgeries. These studies along with others are summarized in Table 2.
Indications for DBE-ERCP in the tabulated articles ranged from abdominal pain, abnormal LFTs, anemia/GI bleed, acute/chronic pancreatitis, cholangitis, and biliary/pancreatic duct dilatation to removal of a previously placed stent, sphincter of Oddi dysfunction type 1, post-cholecystectomy bile leak [27], pancreaticanastamotic stricture, suspected common bile duct stone/stricture, and suspected pancreaticobiliary cancer.
Various factors have been cited as affecting yield in these studies. In the Shah et al.multicenter experience, three-fourths of ERCP failures were related to the inability of the enteroscope to be advanced to the papilla of the pancreaticobiliary-enteric anastomosis [25]. Given such mechanical obstacles, yield can be impacted if the primary end point of the study is therapeutic intervention. For instance, even if cholangiography is achieved but the intended therapeutic intervention is unsuccessful, it may be considered a technical failure. Patel et al. added that diagnostic yield was dependent on the type of altered bowel anatomy and the indication for ERCP, such as biliary versus pancreatic indication [26]. The success rate of DBE-ERCP according to them was much lower for pancreatic indication compared with biliary indication. Along parallel lines Choi et al. opined that DBE-ERCP had a reasonable success rate for managing biliary stone disease but did not adequately address Sphincter of Oddi Dysfunction (SOD) and pancreatic diseases [24]. Note must also be made of the possible advantages afforded by the short DBE system namely better maneuverability, effective pressure application to the enteroscope (increasing the likelihood of reaching the papilla or anastomosis, and allowing the use of commercially available ERCP cannulas), and the use of instruments to intervene therapeutically— benefits which clearly improved the overall success rate/yields in those respective studies.
Additionally, authors urged further evaluation of the role of the endoscopist’s training for complex DBE, technical limitation of the DBE endoscope (increasing accessory channel, incorporating a side-vision optical system, adding an elevator system), and DBE accessories for ERCP (longer pancreaticobiliary stent delivery system) on the diagnostic yield of DBE in patients with surgically altered bowel anatomy.
Overall, DBE-ERCP enabled the ampulla to be reached in 83% (90 of 108 attempts) of the cases, with a diagnostic yield of 77%, and a therapeutic yield of 75%. Time needed to complete the procedure was between 90-134 minutes with minimal complications (3-12% overall).
Dellon et al. initially proved the feasibility of SBE-ERCP in a small case series of patients with prior Roux-en-Y anastomosis [29]. Consequently, larger experiences with SBE-ERCP in patients with Roux-en-Y in the setting of gastric bypass have been published. The findings of these studies are summarized in Table 3.
Indications for SBE-ERCP ran the gamut from the evaluation of abdominal pain with abnormal LFT results and/or biliary ductal dilation, acute/recurrent cholangitis, cholangitis with retained biliary stent after pancreaticoduodenectomy to symptomatic choledocholithiasis with a PTC (Percutaneous TranshepaticCholangiogram) drain in place, pancreatitis secondary to microlithiasis, biliary stricture or ampullary mass, cholestasis, recurrent primary sclerosing cholangitis with strictures, and choledocholithiasis amongst others [30].
While Saleem et al. [31], attributed unsuccessful ERCPs negatively affecting yield to failure to identify the afferent limb of the Roux-en-Y anastomosis, marked bowel loop angulations, inability to enter the afferent limb, and failed cannulation of native papillae, Lennon et al. highlighted that the only factor associated with increasing diagnostic yieldwas operator experience which was associated with a significant increase in diagnostic success rates in SBE-ERCP [32].Dellon et al. reported the time- and labor- intensive (two person procedure) nature of SBE-ERCP and the persistent challenges related to reliably identifying the biliary jejunal limb, stable enteroscope positioning for cannulation, and appropriate accessory devices as probable contributors to yield and success rates [29].Other postulated influencing factors were the type of roux-en-y anatomy, cannulation rates in patients with surgical anastomosis versus native ampulla, and the type of sedation.
Overall, the ampulla was reached in 71% (81 of 114) of the patients/cases when single-balloon enteroscopy assisted ERCP; diagnostic yield of 55% and a therapeutic yield of 81% were achieved. Average time (mean) needed to complete the procedure was between 72-120 minutes with minimal complications (3.5-12.5% overall).
Spiral overtube-assisted ERCP was at the outset reported only as small retrospective case series in abstract form. Wagh and Draganov were the first to publish a prospective evaluation of SE-ERCP in patients with surgically altered anatomy [35]. Thereafter, studies assessing SE-ERCP in RYGB patients were published. These studies are summarized in Table 4.
Indications for SE-ERCP were akin to the other overtube assisted systems:biliary obstruction, bile duct stones, pancreatic duct leaks, abnormal LFTs, cholangitis, abnormal liver enzyme levels, and pancreatitis.
As far as factors affecting yield, Wagh et al. contended that if the papilla/duct enterostomy was reached, cannulation of the desired duct and endoscopic therapy was successful in 90% of the procedures [35]. This observation is in keeping with the Shah et al. multicenter experience, where three-fourths of ERCP failures were related to the inability of the enteroscope to reach the papilla of pancreaticobiliary-enteric anastomosis.
Overall, utilizing SE-ERCP aided access to the ampulla 70% (45 of 64) of the time in RYGB patients. Diagnostic yield of 41% and therapeutic yield of 68% were attained across cases. Mean time required to complete the procedure was 81-120 minutes.
Likewise, Lennon et al. compared single-balloon assisted ERCP and spiral assisted ERCP in patients with Roux-en-Y anatomy in terms of diagnostic and therapeutic yield, procedure time, and complications [32]. They concluded that diagnostic and therapeutic yields are similar with SBE-ERCP and SE-ERCP in patients with Roux-en-Y anatomy with no significant differences in procedure time or complication rates.
As far as comparative studies exploring transoral (e.g. double-balloon) versus surgical approach is concerned, Choi et al. identified 72 RYGB patients who had ERCP via either gastrostomy (GERCP) vs. double balloon enteroscopy [24]. Of the 32 DBE-ERCPs performed, the ampulla was reached 78% of the time with a diagnostic yield of 63% and therapeutic yield of 56%. This was in comparison to 97% across the board (accessing MP, cannulation rate, intervention) for gastrostomy assisted ERCP. The major weakness/downside of GERCP was the complication rate, nearly 5 times (14.5% vs. 3.1%) that of DBE-ERCP.
Similarly, studies like that undertaken by Schreiner et al. have looked at RYGB patients who underwent Laparoscopy-assisted (LA) as opposed to Balloon Enteroscopy-assisted (BEA) ERCP [36]. BEA included single- and double-balloon enteroscopy. Understandably, LA-ERCP was superior to BEA-ERCP in papilla identification and cannulation rate, but data from the retrospective chart review suggested that patients having a Roux + LTJJ (from ligament of Treitz to jejunojenunal anastomosis) limb length less than 150 cm had significantly higher rate of therapeutic success with BEA-ERCP compared with those with Roux + LTJJ limb length 150 cm or longer (88% vs 25%, respectively) and hence the authors recommended it be offered first in these individuals. There was no difference in postprocedure hospital stay or complication rate between the LA-ERCP and BEA-ERCP groups. Univariate and multivariate analysis revealed greater success rate with double-balloon enteroscopy than with single balloon enteroscopy.
Desai et al. has published an analogous study matching spiral enteroscopy versus laparoscopic-assisted endoscopy for completion of ERCP in patients with RYGB surgery [37]. The primary outcome measured was successful cannulation of the bile duct which, was found to be 57% in spiral group vs. 100% in surgical group. However, the conclusion was that if cholangiogram was successful using spiral enteroscopy, there was a decrease in the need for hospitalization, length of stay and total cost. In other words, spiral enteroscopy was deemed to be a potential cost saving alternative in patients with Roux-en-Y anatomy with biliary complications.
The main hurdle as mentioned before has been identifying and traversing the transformed anatomy post RYGB during ERCP. This has been overcome with the help of overtube systems. Currently three are available: double-balloon, single-balloon, and rotational.
Our review, based on recent literature & publications, shows good success rates when comparing ability to reach ampulla (DBE-ERCP: 83%; SBE-ERCP: 71%; SE-ERCP: 70%), diagnostic (DBE-ERCP: 77%; SBE-ERCP: 55%; SE-ERCP: 41%) and therapeutic yields (DBE-ERCP: 75%; SBE-ERCP: 81%; SE-ERCP: 68%)with low complication rates for all three systems. Given these results, the overtube system of choice to be used for a given procedure/ERCP is at the discretion and comfort-level of the endoscopist.
Mention must be made of the “short” DBE system, which measures 152 cm in length and is short enough to let standard length ERCP accessories to be used. The length of the conventional “long” double-balloon enteroscope (200cm) precludes the use of many standard ERCP devices. This makes biliary and pancreatic interventions challenging and time consuming. Another reason why more accessories need to be developed for overtube assisted systems in the future.
In conclusion, our data gives an overview of all three available overtube systems for ERCP in RYGB patients. The current literature supports the use of all overtube-assisted systems. They are effective and safe, with low complication rates. So they need to be considered as a first line modality in RYGB patients requiring ERCP.
References
- American Society for Metabolic and Bariatric Surgery (2009) Fact Sheet: Metabolic & Bariatric Surgery.
- Nguyen NT, Masoomi H, Magno CP, Nguyen XM, Laugenour K, et al. (2011) Trends in use of bariatric surgery, 2003-2008. J Am CollSurg 213: 261-266.
- Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program. American College of Surgeons.
- Nelson DW, Blair KS, Martin MJ (2012) Analysis of obesity-related outcomes and bariatric failure rates with the duodenal switch vs gastric bypass for morbid obesity. Arch Surg 147: 847-854.
- Santry HP, Gillen DL, Lauderdale DS (2005) Trends in bariatric surgical procedures. JAMA 294: 1909-1917.
- Gentileschi P, Kini S, Catarci M, Gagner M (2002) Evidence-based medicine: open and laparoscopic bariatric surgery. SurgEndosc 16: 736-744.
- Melvin WS (2004) Roux-en-Y gastric bypass is the operation of choice for bariatric surgery. J GastrointestSurg 8: 398-400.
- Khashab MA, Okolo PI 3rd (2011) Accessing the pancreatobiliary limb and ERCP in the bariatric patient. GastrointestEndoscClin N Am 21: 305-313.
- Elder KA, Wolfe BM (2007) Bariatric surgery: a review of procedures and outcomes. Gastroenterology 132: 2253-2271.
- Samuel I, Mason EE, Renquist KE, Huang YH, Zimmerman MB, et al. (2006) Bariatric surgery trends: an 18-year report from the International Bariatric Surgery Registry. Am J Surg 192: 657-662.
- ASMBS The Story of Surgery for Obesity. Brief History and Summary of Bariatric Surgery. Chapter 3, Gastric Bypass.
- Upchurch BR, Vargo JJ (2008) Small bowel enteroscopy. Rev GastroenterolDisord 8: 169-177.
- ASGE Technology Committee, Tierney WM, Adler DG, Conway JD, Diehl DL, et al. (2009) Overtube use in gastrointestinal endoscopy. GastrointestEndosc 70: 828-834.
- Ross AS (2009) Endoscopic retrograde cholangiopancreatography in the surgically modified gastrointestinal tract. GastrointestEndoscClin N Am 19: 497-507.
- Haber GB (2007) Double balloon endoscopy for pancreatic and biliary access in altered anatomy (with videos). GastrointestEndosc 66: S47-50.
- Yamamoto H, Sekine Y, Sato Y, Higashizawa T, Miyata T, et al. (2001) Total enteroscopy with a nonsurgical steerable double-balloon method. GastrointestEndosc 53: 216-220.
- Elena RM, Riccardo U, Rossella C, Bizzotto A, Domenico G, et al. (2012) Current status of device-assisted enteroscopy: Technical matters, indication, limits and complications. World J GastrointestEndosc 4: 453-461.
- Kuga R, Safatale-Ribeiro AV, Sakai P, Ishida RK, Faintuch J, et al. (2006) Usefulness of the Double-Balloon Enteroscope for Endoscopic Evaluation of the Bypassed Stomach After Vertical Banded Gastroplasty with Roux-En-Y Gastric Bypass for Morbid Obesity. Gastrointestinal Endoscopy 63: AB 162.
- Emmett DS, Mallat DB (2007) Double-balloon ERCP in patients who have undergone Roux-en-Y surgery: a case series. GastrointestEndosc 66: 1038-1041.
- Siddiqui AA, Chaaya A, Shelton C, Marmion J, Kowalski TE, et al. (2013) Utility of the Short Double-balloon Enteroscope to Perform Pancreaticobiliary Interventions in Patients with Surgically Altered Anatomy in a US Multicenter Study. Digestive Diseases and Sciences 58: 858–864.
- Mehdizadeh S, Ross A, Gerson L, Leighton J, Chen A, et al. (2006) What is the learning curve associated with double-balloon enteroscopy? Technical details and early experience in 6 U.S. tertiary care centers. Gastrointestinal Endoscopy 64: 740-750.
- Moreels TG, Hubens GJ, Ysebaert DK, Op de Beeck B, Pelckmans PA (2009) Diagnostic and therapeutic double-balloon enteroscopy after small bowel Roux-en-Y reconstructive surgery. Digestion 80: 141-147.
- Kuga R, Furuya CK Jr, Hondo FY, Ide E, Ishioka S, et al. (2008) ERCP using double-balloon enteroscopy in patients with Roux-en-Y anatomy. Dig Dis 26: 330-335.
- Choi EK, Chiorean MV, Coté GA, El Hajj II, Ballard D, et al. (2013) ERCP via gastrostomy vs. double balloon enteroscopy in patients with prior bariatric Roux-en-Y gastric bypass surgery. SurgEndosc 27: 2894-2899.
- Shah RJ, Smolkin M, Yen R, Ross A, Kozarek RA, et al. (2013) A multicenter, U.S. experience of single-balloon, double-balloon, and rotational overtube-assisted enteroscopy ERCP in patients with surgically altered pancreaticobiliary anatomy.GastrointestEndosc 77: 593-600.
- Patel MK, Horseley-Silva J, Gómez V, Stauffer JA, Stark ME, et al. (2013) Double Balloon Enteroscopy Procedure in Patients with Surgically Altered Bowel Anatomy: Analysis of a Large Prospectively Collected Database. J Laparoendosc&Adv Surgical Techniques 23: 409-413.
- Gutierrez JP, Smith IB, Wilcox CM, Mönkemüller K (2013) Bile leak from the duct of Luschka treated with double-balloon enteroscopy ERCP in a patient with Roux-en-Y gastric bypass. Endoscopy 45 Suppl 2 UCTN: E404.
- Di Caro S, May A, Heine DG, Fini L, Landi B, et al. (2005) The European experience with double-balloon enteroscopy: indications, methodology, safety, and clinical impact. GastrointestEndosc 62: 545-550.
- Dellon ES, Kohn GP, Morgan DR, Grimm IS (2009) Endoscopic retrograde cholangiopancreatography with single-balloon enteroscopy is feasible in patients with a prior Roux-en-Y anastomosis. Dig Dis Sci 54: 1798-1803.
- Wang AY, Sauer BG, Behm BW, Ramanath M, Cox DG, et al. (2010) Single-balloon enteroscopy effectively enables diagnostic and therapeutic retrograde cholangiography in patients with surgically altered anatomy. GastrointestEndosc71: 641.
- Saleem A, Baron TH, Gostout CJ, Topazian MD, Levy MJ, et al. (2010) Endoscopic retrograde cholangiopancreatography using a single-balloon enteroscope in patients with altered Roux-en-Y anatomy. Endoscopy 42:656.
- Lennon AM, Kapoor S, Khashab M, Corless E, Amateau S, et al. (2012) Spiral assisted ERCP is equivalent to single balloon assisted ERCP in patients with Roux-en-Y anatomy. Dig Dis Sci 57: 1391-1398.
- Akerman PA, Cantero D (2009) Spiral enteroscopy and push enteroscopy. GastrointestEndoscClin N Am 19: 357-369.
- Kogure H, Watabe H, Yamada A, Isayama H, Yamaji Y, et al. (2011) Spiral enteroscopy for therapeutic ERCP in patients with surgically altered anatomy: actual technique and review of the literature. J HepatobiliaryPancreatSci 18: 375-379.
- Wagh MS, Draganov PV (2012) Prospective evaluation of spiral overtube-assisted ERCP in patients with surgically altered anatomy. GastrointestEndosc 76: 439-443.
- Schreiner MA, Chang L, Gluck M, Irani S, Gan SI, et al. (2012) Laparoscopy-assisted versus balloon enteroscopy-assisted ERCP in bariatric post-Roux-en-Y gastric bypass patients. GastrointestEndosc 75: 748-756.
- Desai SV, Naveed M, Jazwinski A, Jowell PS, Branch MS (2011) Spiral Enteroscopy Versus Laparoscopic-Assisted Endoscopy for Completion of ERCP in Patients With Roux-en-Y Gastric Bypass Surgery.GastrointestEndosc. 73: AB122.
- Wright BE, Cass OW, Freeman ML (2002) ERCP in patients with long-limb Roux-en-Y gastrojejunostomy and intact papilla. GastrointestEndosc 56: 225-232.
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 15311
- [From(publication date):
September-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 10700
- PDF downloads : 4611
