Research Article Open Access
Treatment Approach to Infant with Sepsis and Neurological Complications Resulting in Multicystic Encephalomalacia
Mirla Fiuza Diniz*, Rayanna Mara De-Oliveira Santos Pereira and Leonardo Brandão Barreto
Escola de Medicina – Universidade Federal de Ouro Preto, Brazil
- *Corresponding Author:
- Mirla Fiuza Diniz
Escola de Medicina – Universidade
Federal de Ouro Preto, Brazil
Tel: 55 31 3559-1189
E-mail: mirladiniz_13@hotmail.com
Received date: July 24, 2017; Accepted date: August 08, 2017; Published date: August 10, 2017
Citation: Diniz MF, Santos Pereira RMD, Barreto LD (2017) Treatment Approach to Infant with Sepsis and Neurological Complications Resulting in Multicystic Encephalomalacia. J Neuroinfect Dis 8:260. doi:10.4172/2314-7326.1000260
Copyright: © 2017 Diniz MF, et al. This is an open-access article distributed under the terms of the creative commons attribution license, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Background: Destructive brain lesions result from aggression to the central nervous system and can be congenital or acquired in the postnatal period. When extensive, these lesions can produce cavitations, as in multicystic encephalomalacia (MCE). The most common etiology of MCE is neonatal hypoxia and ischemia, but there are reports of cases due to viral encephalopathies and head traumas. MCE has a poor prognosis, usually resulting in severe neurological sequelas or death. This article reports a case of multicystic encephalomalacia in the Santa Casa de Misericordia de Ouro Preto-MG (Brazil) contrasting its etiology with those found in the literature as well as discussing the treatment approach to the patient.
Case report: A 10-month-old child, born full-term, hospitalized since birth for treatment of sepsis of pulmonary focus evolved with fungal sepsis and supratentorial hydrocephaly leading to the implantation of a ventricular shunt. As the patient developed ventriculitis, the catheter was removed. Polymyxin B was administered intrathecally and lumbar punctures were performed to relieve the hydrocephaly. The patient maintained the alterations in the liquor exam, despite the prolonged antibiotics therapy and had multiple cystic lesions, intra and extra-ventricular, with a compressive aspect, and residual brain parenchyma on the CT, characterizing MCE. The patient passed away after a few weeks of further care and no improvement on overall status.
Discussion: MCE results from a brain lesion at the end of pregnancy, during birth or in the perinatal period, and it leads to the formation of poorly defined cavities with glial reaction creating septa. The etiologies presented by the patient of fungal and bacterial infection weren't common in the literature.
Conclusion: The administration of a larger spectrum antibiotic and the reimplantation of the ventricular shunt could possibly have prevented the progression of the hydrocephaly and the evolution of the case to MCE.
Keywords
Multicystic encephalomalacia (MCE); Sepsis
Introduction
Destructive brain lesions can result from any aggression to the central nervous system and may be congenital or acquired during the postnatal period [1,2]. Several factors may be involved in their etiology, including infections [3,4]. When extensive, these lesions produce destruction of brain tissue and formation of cavities, such as multicystic encephalomalacia (MCE), which is characterized by the presence of cystic cavities that can reach all the hemispheric white matter and even the cortex [5], establishing itself before or after birth. MCE results from a brain lesion at the end of pregnancy, during birth or in the perinatal period and is related to hypoxic-ischemic states, viral encephalitis and head traumas [6,7].
We aim to report a case of multicystic encephalomalacia (MCE) with massive cell necrosis in an infant with previous fungal and bacterial sepsis.
Material and Methods
Based on a case report from the Santa Casa de Misericórdia de Ouro Preto in Ouro Preto-MG (Brazil) and a brief literary review during 2009-2012, we contrasted data on the etiology of MCE in newborns and children. The bibliographic references were obtained from Pubmed and the Web of Knowledge and the key words used were: encephalopathy, multicystic encephalomalacia and their correspondents.
Results and Discussion
A 10-month-old female infant, born full-term and hospitalized since birth for treatment of early-onset neonatal sepsis of pulmonary focus, evolved with secondary fungal sepsis and presented an increase in the cephalic perimeter. A head computerized tomography evidenced supratentorial hydrocephalus and the patient was referred for surgical treatment. She was submitted to implantation of a ventricular catheter but evolved with ventriculitis that required withdrawal of the catheter and prescription of intrathecal polymyxin B plus intravenous meropenem, vancomycin and amikacin.
There was a period of instability with decompensation of hydrocephalus and changes in the respiratory pattern, controlled with relief lumbar punctures. She then presented stability of the respiratory pattern and compensation of hydrocephalus, with maintenance of altered values on the cerebrospinal fluid despite prolonged antibiotic therapy. The patient remained afebrile, awake, hyperactive to the stimulus, with stable neurological pattern, no episodes of emesis, no need of oxigen supplementation, spontenous movement of limbs and no other changes or stigmas.
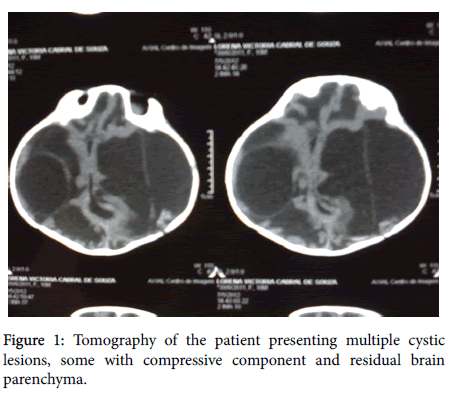
Computer head tomography created brain images in a multislice device, with axial reconstruction of 2.0 mm and 5.0 mm thickness, without intravenous injection of contrast medium. There was significant reduction of the encephalic tissue, with the remaining tissue being significantly compressed by intra- and extra-ventricular cystic formations. There was also a marked increase in the dimensions of the IV ventricle, cranial deformity and craniofacial disproportion, with sutures being diffusely open (Figure 1). No calcifications were identified in the remaining brain tissue. These features are compatible with the sequelae of the inflammatory/infectious process.
Despite the initial stability, after a few more weeks of care, the patient passed away.
Conclusion and Final Considerations
When brain lesions are extensive they produce destruction of brain tissue and formation of cavities, as in the MCE. The multicystic nature of MCE has been mainly associated to viral encephalitis, but can also occur in hypoxic-ischemic states. The etiologies presented by the patient seen in our service were not common in literary publications.
The administration of a larger spectrum antibiotic and the reimplantation of the ventricular shunt could possibly have prevented the progression of the hydrocephaly but MCE traditionally has a poor prognosis regardless of care, usually resulting in severe neurological sequalae.
References
- Frigieri G, Guidi B, Zaccarelli SC, Rossi C, Muratori G, et al. (1996) Multicystic encephalomalacia in term infants. Childs Nervous System 12: 759-764.
- Karaman E, Isildak H, Yilmaz M, Enver O, Albayram S (2011) Encephalomalacia in the frontal lobe: Complication of the endoscopic sinus surgery. J Craniofac Surg 22: 2374-2375.
- Low C, Garzon E, Carrete H, Vilanova LC, Yacubian EM, et al. (2007) Early destructive lesions in the developing brain: Clinical and electrographic correlates. Arq Neuropsiquiatr 65: 416-422.
- Matlung SE, Bilo RAC, Kubat B, Van Rijn RR (2011) Multicystic encephalomalacia as an end-stage finding in abusive head trauma. Forensic Sci Med Pat 7: 355-363.
- Kinney HC, Haynes RL, Xu G, Andiman SE, Folkerth RD, et al. (2012) Neuron deficit in the white matter and subplate in periventricular leukomalacia. Ann Neurol 71: 397-406.
- Funayama CAR, Ferlin MLS, Bellucci AD (1997) Convulsões neonatais - Relato de caso. Medicina, Ribeirão Preto 30: 268-271.
- Huang ZH, Sun Y, Chen C (2011) Progress in encephalopathy of prematurity. Zhongguo Dang Dai Er Ke Za Zhi 13: 771-775.
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 5320
- [From(publication date):
September-2017 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 4444
- PDF downloads : 876