Case Report Open Access
A Typical Extramedullary Haematopoiesis in a JAK2 Mutated Primary Myelofibrosis Patient after a Minor Head Injury
| Vadsala Baskaran1*, Cho Wai Sum1, Mansoor Aslam2, Alfredo Addeo3 and Ciro Roberto Rinaldi1 | |
| 1Department of Haematology, United Lincolnshire Hospitals NHS Trust (ULHT), Boston, UK | |
| 2Department of Radiology, United Lincolnshire Hospitals NHS Trust (ULHT), Boston, UK | |
| 3Department of Oncology, United Lincolnshire Hospitals NHS Trust (ULHT), Boston, UK | |
| Corresponding Author : | Vadsala Baskaran Department of Haematology United Lincolnshire Hospitals NHS Trust (ULHT), Boston, UK E-mail: reksha_01@yahoo.com |
| Received January 27, 2013; Accepted March 26, 2013; Published March 28, 2013 | |
| Citation: Baskaran V, Sum CW, Aslam M, Addeo A, Rinaldi CR (2013) Atypical Extramedullary Haematopoiesis in a JAK2 Mutated Primary Myelofibrosis Patient after a Minor Head Injury. OMICS J Radiology 2:114. doi: 10.4172/2167-7964.1000114 | |
| Copyright: © 2013 Baskaran V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Intracranial extramedullary haematopoiesis (EMH) is very rare. We report the case of EMH with intracranial involvement which developed after trauma in a 73-year-old lady affected by JAK2 mutated myelofibrosis (MF). She was diagnosed with MF in 2005 and treated with low-dose-steroids (prednisolone and oxymethalone) for about 5 years with anexcellent response on full blood count and splenomegaly.
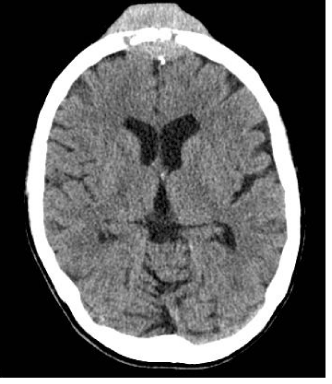
In June 2011, she fell from the stairs and sustained minor trauma to the forehead. Six weeks later, the patient had a gradually enlarging and moderately painful lump in the centre of her forehead. A contrast-enhanced CT scan of the head was performed, showing a small fracture in the frontal bone infiltrated and surrounded by a soft tissue mass extending intracranially and invading the skin extracranially (Figures 1 and 2). A metastatic deposit from an occult tumour was suspected.
In August 2011, we performed a CT-guided trucut biopsy of the forehead mass. The histology report confirmed extramedullary haematopoiesis according to the patchy expression of myeloid (CD45, CD43, myeloperoxidase) and megakaryocytic markers (CD68, CD42b). We concluded that the trauma caused a small fracture which triggered the bone marrow tissue reaction resulting in production of extramedullary haematopoiesis in the site of the trauma. The patient underwent local radiotherapy resulting in complete resolution of the lesion.
| Background |
| Extramedullary haematopoiesis (EMH) is defined as the proliferation of haematopoietic cells outside of the bone marrow cavity in response to chronic haematological stress. It is a compensatory process associated with either bone marrow replacement disease (myelofibrosis or chronic myelogenous leukemia) or haemolytic anemia (thalassemia, sickle cell anemia, or hereditary spherocytosis) [1]. |
| EMH mainly involves the reticuloendothelial system (liver, spleen, and lymph nodes) but is also known to occur in the thyroid, prostate, pericardium, kidney and lungs [2]. Intracranial haematopoiesis is rare and most frequently reported causes are thalassemia (50%) and myelofibrosis (31%) [3]. Our case demonstrates trauma induced EMH with intracranial involvement in myelofibrosis. |
| Rong Li et al. highlighted that EMH occurring following a traumatic event is very rare and has been observed in the presacral area following sacrum fracture and lung tissue following bone fracture or cardiac surgery [4]. In our case, the skull fracture is thought to have triggered bone marrow tissue reaction (tissue inflammation, injury and repair) resulting in production of EMH in the site of the trauma. |
| Radiation therapy has proven to be a very effective modality for treatment of this rare disease which is exquisitely radiosensitive [5]. A total radiation dose in the range of 10–25 Gy usually induces a durable remission and improvement of symptoms [5]. In our case, 25 Gy divided in 2.5 Gy fractions were used effectively with complete resolution of symptoms. |
| Case Presentation |
| This 73 year-old lady who was previously fit and well was diagnosed with chronic idiopathic myelofibrosis in 2005. Polymerase chain reaction (PCR) of the peripheral blood confirmed JAK2 mutation. She was treated with low dose steroids (Prednisolone and Oxymethalone) with excellent response where the massive splenomegaly reduced from 16cm to 9cm within the first month and blood count remained stable. |
| In June 2011, she fell down the stairs at home and sustained minor trauma to the forehead with some bruising but she was otherwise comfortable without any pain. Six weeks later, the patient had a gradually enlarging and moderately painful lump in the centre of her forehead. She was admitted via the Emergency Department with headache and a palpable mass of 6×4 centimetres in size, centrally over the frontal region. |
| A computed Tomography (CT) scan of the head with contrast was performed and revealed a small fracture in the frontal bone which was infiltrated and surrounded by a soft tissue mass extending intracranially and invading the skin extra cranially (Figures 1 and 2). Differential diagnosis included dural metastasis from unknown primary, lymphoma, meningiomatosis and neurosarcoidosis. However, a subsequent full body CT showed no other mass lesions and tumour markers were negative. Further investigation with bone scintigraphy showed increased uptake in the forehead lesion and right mid-femur which was atypical for bone metastasis, therefore extramedullary haematopoiesis was considered as a possible diagnosis. |
| In August 2011, a CT-guided trucut biopsy of the forehead mass was performed. The sample was sent to Nottingham University Hospitals Trust for expert opinion. The overall appearance was thought to represent EMH given the patchy expression of some myeloid (CD45, CD43, myeloperoxidase) and megakaryocytic markers (CD68, CD42b). |
| Following the diagnosis of EMH, the patient was referred to clinical oncology for palliative radiotherapy. She completed two-week course of radiotherapy (10 fractions) with significant reduction in pain and swelling. Follow up a month later showed that the mass on the forehead had completely resolved apart from irregularity of the skull which was discernible on palpation. She would most likely have a permanent bony deformity of the forehead due to significant distortion of the frontal bone previously despite having good response of the mass to radiotherapy. |
References |
|
--
Figures at a glance
 |
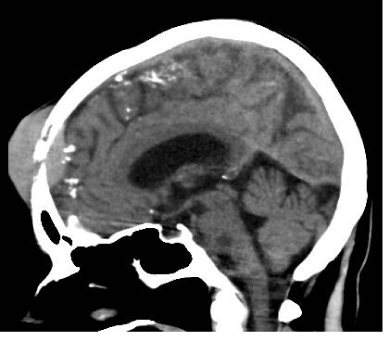 |
| Figure 1 | Figure 2 |
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 14858
- [From(publication date):
April-2013 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 10139
- PDF downloads : 4719
