Research Article Open Access
Lumbar Percutaneous Intradiscal Injection of Radiopaque Gelified Ethanol (Discogel) in Patients with Low Back and Radicular Pain
| Volpentesta G1, De Rose M1, Bosco D3, Stroscio C1, Guzzi G1, Bombardieri C2, Chirchiglia D1, Plastino M3, Romano M1, Cristofalo S3, Pardatscher K2 and Lavano A1* | |
| 1 Department of Neurosurgery, University Hospital of Germaneto, Campus “Salvatore Venuta”, Catanzaro, Italy | |
| 2 Department of Neuroradiology, University Hospital of Germaneto, Campus “Salvatore Venuta”, Catanzaro, Italy | |
| 3 Department of Neurology, “San Giovanni di Dio” General Hospital, Crotone, Italy | |
| Corresponding Author : | Lavano A Department of Neurosurgery University Hospital of Germaneto Campus “Salvatore Venuta”, Viale Europa 88100 Catanzaro, Italy Tel: +3909613647385 E-mail: lavano@unicz.it |
| Received April 04, 2014; Accepted April 27, 2014; Published April 29, 2014 | |
| Citation: Volpentesta G, De Rose M, Bosco D, Stroscio C, Guzzi G, et al. (2014) Lumbar Percutaneous Intradiscal Injection of Radiopaque Gelified Ethanol (“Discogel”) in Patients with Low Back and Radicular Pain. J Pain Relief 3:145. doi: 10.4172/2167-0846.1000145 | |
| Copyright: © 2014 Volpentesta G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Partial removal of nucleus pulposus with consequent reduction of intradiscal pressure may be obtained with percutaneous intradiscal administration of chemical substances in the intervertebral disc. We used percutaneous intradiscal injection of radiopaque gelified ethanol (“Discogel”) in 72 patients (group 1) with conservative treatment resistant lumbar and radicular pain due to small and medium-size hernias of intervertebral disc to demonstrate its efficacy and safety vs. 72 subjects treated with intra-foraminal and intradiscal injections of a steroid and anesthetic (group 2 or control group). “Discogel” injection was performed with biplane fluoroscopy assistance and under local anesthesia with patient in lateral position on symptomatic side. Amount of “Discogel” injected ranged from 0.8 ml to 1.6 ml. We treated a total of 83 discs. We performed the procedure on one disc in 62 patients; in 9 patients two discs were treated in the same session and in 1 patient three levels were treated in two separate sessions. In group 1 patient “responders” were 65 (90.3%). Excellent and good results were obtained in 58 patients (80.4%), satisfactory results in 7 patients (9.8%) and poor results in 7 patients (9.8%); among “responders” pain control was quite immediate in 58 patients (89.3%) while in 7 patients (10.7%) there was a delay of 7-10 days. These values were significantly higher than in control group. Also the quality of life was significantly more sustained vs. control group, and this benefit was maintained over time. Concerning complications, in 3 cases (4.15%) we had transitory radicular irritation with neuropathic pain appearance immediately after the procedure and in 1 case (1.30%) transitory sensory-motor deficit due to diffusion of local anesthetic along the introducer needle. In conclusion intradiscal radiopaque gelified ethanol injection is minimally invasive, low cost, safe and effective procedure that may be considered in proper selected patients before recourse to surgery.
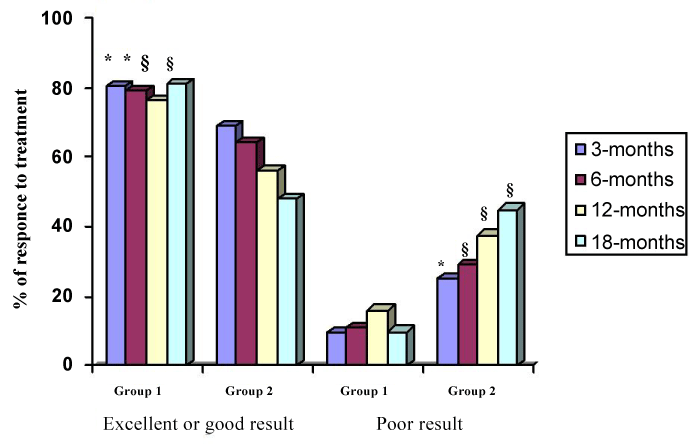
In group 1 patient “responders” were 65 (90.3%). Excellent and good results were obtained in 58 patients (80.4%), satisfactory results in 7 patients (9.8%) and poor results in 7 patients (9.8%); among “responders” pain control was quite immediate in 58 patients (89.3%) while in 7 patients (10.7%) there was a delay of 7-10 days. These values were significantly higher than in control group. Also the quality of life was significantly more sustained vs. control group, and this benefit was maintained over time. Concerning complications, in 3 cases (4.15%) we had transitory radicular irritation with neuropathic pain appearance immediately after the procedure and in 1 case (1.30%) transitory sensory-motor deficit due to diffusion of local anesthetic along the introducer needle.
In conclusion intradiscal radiopaque gelified ethanol injection is minimally invasive, low cost, safe and effective procedure that may be considered in proper selected patients before recourse to surgery.
We assessed the therapeutic outcome of percutaneous intradiscal injection of radiopaque gelified ethanol (Discogel) and compared the outcome of intra-foraminal and intradiscal injections of a steroid and an anesthetic in the management of radicular pain related to lumbar disk herniation.
After treatments patients were evaluated by neurosurgeon assigned to follow-up that was not the same who performed procedures and who was not aware of type of procedures made. In both groups follow-up was carried out at 1, 3, 6 months, 12 months and 18 months, assessing pain intensity on VAS scale, limitation on physical activity and HRQoL on SF-36 score. In group 2 also CT scan was performed at 1, 3 and 6 months after the surgery to assess the anatomic changes of the treated discs. The response to treatment was classified as: a. excellent result (pain totally disappeared, full recovery of physical activity); b. good result (pain improvement on the VAS score > 70%, no limitation on physical activity); c. satisfactory result (pain improvement on the VAS score > 50%, moderate limited physical activity); d. poor result (pain improvement on the VAS score < 50%, very limited physical activity).
Among the “responders” low back pain improvement was quite immediate (on the day of the procedure or on the day after) in 58 patients (89.3%) while in 7 patients (10.7%) there was a delay of 7-10 days; improvement of radicular pain was obtained in a period of 2 to 3 weeks.
At the beginning of the “Discogel” injection the majority of patients felt a heat sensation at the level of the injected disc that disappeared at the end of the procedure, probably due to irritation of the intersomatic disc nerve endings.
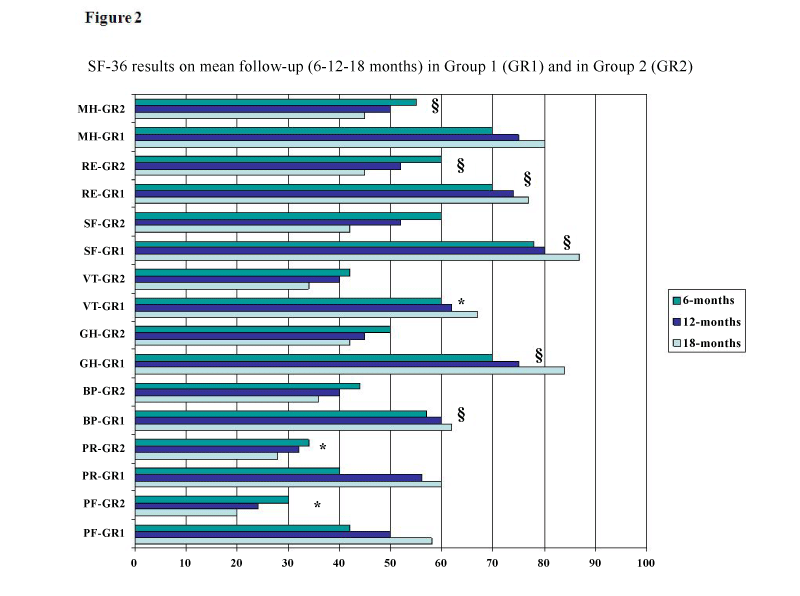
In 3 cases (4.15%) a radicular irritation with neuropathic pain appearance was evident immediately after the procedure. This condition was due to an excessive epidural leakage of the product with irritation of nerve-endings and improved within 10 days with steroidal anti-inflammatory therapy. In 1 case (1.30%) we observed a transitory sensory-motor deficit due to the diffusion of local anesthetic along the introducer needle: the deficit disappeared within 8 hours. No allergic complications were observed. Pain control was insignificantly unchanged at the 6, 12, 18 months follow-up (Figure 1). Also SF-36 QoL score improved significantly during the follow-up vs. group 2 (Figure 2). On CT scan performed at 1 and 3 months an iperdensity image of “Discogel” was always evident in treated disc without modification of hernia volume; iperdensity image was still evident on CT scan performed at 6 months only in 10 of treated discs and reduction of hernia volume was documented in all “responders”.
- In group 2, after 3-months of follow-up the treatment was a successful in 50 patients (69%; CI: 62%-74.4%); in the remaining 22 patients (30%; CI: 24.6%-34.5%) it failed. Among patients whose treatment was a successful, the outcome was excellent in 34 (47%) and good in 16 (22%). In group 1, among patients whose treatment failed, this was poor in 22 (30%) patients with recourse to surgery in 4 (5%). During or after the treatment, no major or minor complications were observed. Of the 50 patients with excellent benefit to the pharmacological treatment, three (4%) reported a rise of pain after 6-months, 9 (12.5%) after 12-months and 14 patients (19.9%) after 18-months, respectively (Figure 1). SF-36 QoL score showed initial improvement that was reduced in subsequent evaluations (6, 12 and 18-months) (Figure 2).
- Group 1 and group 2 comparison: the statistical analysis with X²-test showed different outcome in every time of evaluation (1, 3, 6, 12 and 18 months). A multiple regression analysis was performed entering treatment type (pharmacological or Discogel) as dependent variable, and VAS-score as independent variables because the latter was alone significantly correlated with type of treatment in univariate analysis (r=0.17; P=0.001). We assessed, also as independent variables, potential confounders known to be risk factors for disc disease.
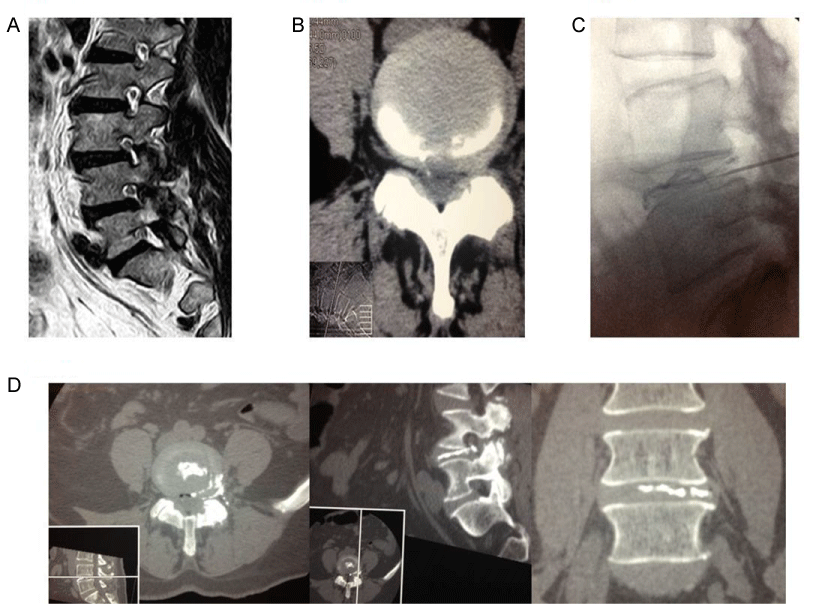
Internal Disc Disruption leads to the “discogenic pain”, characterized by diffuse, dull ache or deep-seated, burning, lancinating pain in the low back with not uncommon irradiation into the leg as referred pain without nerve root entrapment. The pathophysiological mechanism consists of annulus tears, in-growth of granulation tissue and of nociceptive nerve endings, irritation by chemical materials inside the disc or from the epidural area and mechanical stimulation associated with lumbar movement on the sinuvertebral nerve ending distributed in the outer one-third of the annulus and posterior longitudinal ligament. About 39% of all patients with chronic low back pain have IDD. At present the diagnosis of discogenic pain is fundamentally based on the typical symptoms, images on MRI (“black disc” and middle annulus fibrosus bulge) and results of discography that became the main diagnostic criteria. Most patients suffering from discogenic pain show positive in discography and express the similar or exact pain as usual, including quality, location and severity, but sometimes there are some exceptions. Current therapeutic approaches include pharmacologic pain control, minimal invasive interventional procedures on the disc and lumbar interbody fusion [11,12] (Figure 3).
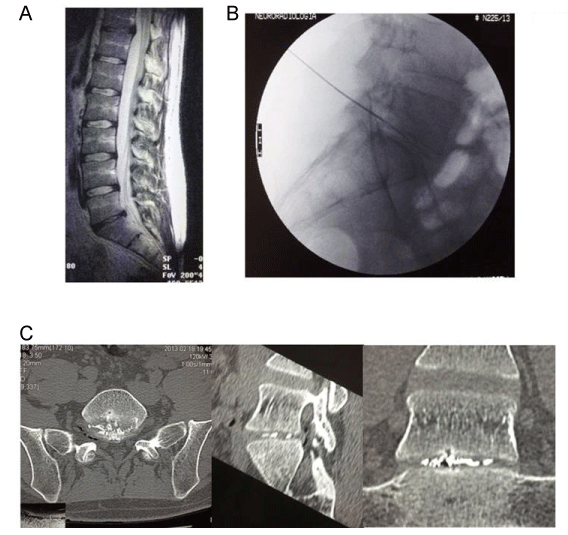
Herniation of lumbar intervertebral disc is the most common cause of low back pain with classical predominantly irradiation along the nerve route course. The process of annular ruptures, disc herniation and nerve root compression can result in a complex picture of symptoms and signs that represents a combination of somatic pain from the outer annulus and posterior longitudinal ligaments and neuropathic radicular pain from nerve root compression together with chemical reaction. In this study, we investigated the therapeutic outcome of percutaneous intradiscal injections of radiopaque gelified ethanol (Discogel) (group 1) vs intraforaminal and intradiscal injections of a steroid and an anesthetic (group 2) in 144 patients with lumbar disc herniation. In group 1, over ninety percent of patients showed excellent or good result that substantially maintained unchanged during follow-up. These percentages were significantly higher than those reported in group 2. Rihn et al., in a recent study, showed that obesity realized less clinical benefit from both operative and non-operative treatment in 336 obese patients with lumbar disc herniation. Nevertheless, in our patients after adjustment for BMI the benefit of Discogel treatment remained strongly significant [13] (Figure 4).
Surgery is considered the treatment of choice for extruded, migrated hand free fragment herniated disc and absolute indication in presence of hyperalgic sciatalgia, sphincteral deficit and progressive neurological deficits.
The possible suboptimal results of surgery and its complications lead to the development of minimally invasive ablative percutaneous techniques that could be offered as alternative to surgical treatment [14]. These techniques are image-guided procedures based on the puncture of the annulus with a trocar: through this trocar chemical, thermal or mechanical ablative device may be placed inside the nucleus pulposus [5,15]. These procedures seem to have established a new concept of “alternative intermediate therapy” [16] in treatment of lumbar herniation. The most relevant agent used in the past for chemical percutaneous technique was Chymopapain. The effectiveness of chemonucleolysis with this enzyme has been widely documented [6,17]. Nevertheless possible side effects and complications as major pain after treatment, systemic allergic reactions, chemical discitis and transverse myelitis [18], leaded to the necessity of new chemonucleolytic substance. However 96%, pure ethanol was used with good results [4]: alcohol produces a molecular scission of proteoglycans and glucosaminoglycans of the nucleus pulposus and consequently a chemical decompression of the disc [19]. Pure ethanol is difficult to handle due to its ready diffusion into the tissues. It indiscriminately attacks annulus, cartilage, vessel, root and dura: discography must be performed before inject ethanol to determine degree of disc degeneration and leakage of contrast into the epidural space, vascular and intraosseus areas; furthermore it cannot be visualized on fluoroscopy.
“Discogel” is a viscous solution consisting in ethanol mixed with ethyl cellulose and tungsten (radiopaque gelified ethanol) that causes a local necrosis of nucleous pulposus and dehydration of the turgescent and protruding disc; thus resulting in retraction of intervertebral disc herniation.
The use of the ethyl cellulose increases the viscosity limiting the ethanol diffusion in the disc and performs a simultaneous deposition of a part of the gel which precipitates making a kind of soft intradiscal “prosthesis”. The tungsten makes the product radiopaque and the amount of gel injected can be monitored with fluoroscopy. The distribution of the product in the axial plane therefore became apparent on CT examination and of major interest is the visualization of the fissures of the annulus and the migration of the product into the symptomatic hernia. The viscosity of gelified ethyl alcohol depends on temperature. Administration of the product warmed up above room temperature should be avoided because the gel becomes more liquid and is below optimum viscosity. In an experimental study Guarnieri [14] showed that “Discogel” produces no morpho-structural changes in the nuclear tissue and annulus and in contact with nervous structure.
The pathogenesis of low back and radicular pain in presence of a herniated disc is multifactorial: it is characterized by mechanical factors, direct or indirect, and by associated inflammatory factors, cell-mediated inflammatory reaction and bio-humoral immunological response. Direct mechanical factors are direct compression of herniated disk on the spinal ganglion and mechanical deformation of posterior longitudinal ligament and annulus with nociceptor stimulation of the recurrent nerve of Lutschka. Indirect mechanical factors are ischemia due to compression on afferent arterioles and nerve bundle microcirculation with anoxic demyelination and venous stasis. Neural inflammation is also important: it is due to autoimmune cell-mediated response to proteoglycans of the herniated fragment and to bio-humoral immunological response due to prostaglandin (PGE2) and leucotrieni produced by phospholipase A2 from arachidonic acid, matrix metalloproteinase (MMP-1-2-2-9), IL-1, IL-6, TNF-alfa. Low back and radicular pain improvement after the intradiscal “Discogel” injection may be due to the dehydration of nucleus pulposus with reduction of intradiscal pressure and retraction of the disc herniation. According with Theron [3] we believe that the most important intradiscal therapeutic reaction is not the immediate reduction of the hernia volume but the decrease of the intradiscal pressure allowing a partial decompressive shift of the herniated nucleus: in our study this is well evidenced by the discordance between the rapid improvement of clinical symptoms and the radiologic image of unchanged volume of disc herniation on CT scan at 1 and 3 months after “Discogel” injection. It is also conceivable a direct effect of ethanol on the disc pain receptors by turning out the nervous endings. Coppes [20] and Freemont [19] demonstrated the presence of nerve fibers into the inner layers of the annulus fibrosus and in the nucleus pulposus in degenerative painful discs and not in normal discs.
Theron [3] reported a success rate of 91.4% in a group of 221 patients with lumbar disc hernias and a complication rate <0.5%, while Stagni [21] a therapeutic success in 24 out of 32 treated patients (75%) without complications. Complications described for the use of Discogel are systemic allergic reactions to the substance, discitis and neurologic injury. In our series we obtained pain improvement > 50% in 90.3% of cases and only few transitory complications: 1 sensory-motor deficit and 3 appearance of neuropathic pain.
Our study has some limitations: first of all this was an observational open-label study; another limitations is the small sample of patients. Still the evaluation was complete and accurate in all patients and performed by a physician experienced in this issue.
References
- McGirt MJ, Ambrossi GL, Datoo G, Scubba DM (2009) Recurrent disc herniation and long-term back pain after primary lumbar discectomy. Neurosurgery 64: 338-344.
- Schofferman J, Reynald J, Herzog R, Convington E, O’Neil C (2003) Failed Back Surgery: etiology and diagnostic evaluation. Spine J 3: 400-403.
- Theron J, Guimaraens L, Casasco A (2007) Percutaneous treatment of lumbar intervertebral disk hernias with radiopaque gelified ethanol: a preliminary study. J Spinal Disord Tech 20: 526-532.
- Riquelme C, Musacchio M, Mont’Alverne F, Tournade A (2001) Chemonucleolysis of lumbar disc herniation with ethanol. J Neuroradiol 28: 219-229.
- Kelekis A, Filippiadis D, Martin JB, Brountzos E (2010) Standards of practice: quality assurance guidelines for percutaneous treatments of intervertebral disc. CardiovascIntervenRadiol 33: 909-913.
- Cardoso Couto JM, Ayres de Castilho E, Rossi Menezes P (2007) Chemonucleolysis in lumbar disc herniation: a meta-analysis. Clinics 62: 175-180.
- Montgomery AS, Asberg M (1979) A new depression scale designed to be sensitive to change. Br J Psychiatry 134: 382-389.
- Mysliwiec LW, Cholewicki J, Winkelpleck MD, Eis GP (2010) MSU Classification for herniated lumbar disc on MRI: toward developing objective criteria for surgical selection. Eur Spine J 19: 1087-1093.
- Downie WW, Leatham PA, Rhind VM, Wright V, Branco JA, et al. (1978) Studies with pain rating scales. Ann Rheum Dis 37: 378-381.
- Melzack R (1987) The short-form McGill Pain Questionnaire. Pain 30: 191-197.
- Sehgal N, Fortin JD (2000) Internal Disc Distruption and low back pain. Pain Physician 3: 143-157.
- Takahashi K, Aoki Y, Ohtori S (2008) Resolvindiscogenic pain. Eur Spine J 17: S424-S431.
- Rihn JA, Kurd M, Milibrand AS, Lurie J, Zhao W, et al. (2013) The influence of obesity on the outcome of treatment of lumbar disc herniation: analysis of the Spine Patients Outcomes Research Trial (SPORT). J Bone Joint Surg Am 95: 1-8.
- Guarnieri G, Vassallo P, Peluzzo MG, Laghi F, Muto M (2009) A comparison of minimally invasive techniques in percutaneous treatment of lumbar herniated disc. Neuroradiol J 22: 108-121.
- Boswell MV, Trescot AM, Datta S, Schultz DM,Hansen HC, et al. (2007) Interventional techniques: evidence-based practical guidelines in the management of chronic pain. Pain Physician 10: 7-111.
- Chiba K (1993) Experimental study on the pathological changes of the intervertebral disc and its surrounding tissues after intradiscal injection of various chemical substances. Nihon SeikeigekaGakkaiZasshi 67: 1055-1069.
- Brown MD (1996) Update on Chemonucleolysis. Spine 21: 625-685.
- Nordby EJ, Wright PH, Schofield SR (1993) Safety of chemonucleolysis: adverse effects reported in USA 1982-1992. ClinOrthopRelat Res 293: 122-134.
- Freemont AJ, Peacock TE, Goupille P, Hoyland JA, O’ Brien J, et al. (1997) Nerve in growth into diseased intervertebral disc in chronic back pain. Lancet 350: 178-181.
- Coppes MH, Marani E, Raph TWM, Thomeer RT, Groen GJ (1997) Innervation of painful lumbar discs. Spine 22: 2342-2349.
- Stagni S, De Sanctis F, Cirillo L, Dall’Olio M, Princiotta C, et al. (2012) A minimally invasive treatment for lumbar disc herniation: DiscoGelchemonucleolysis in patients unresponsive to chemonucleolysis with Oxygen-Ozone. IntervNeuroradiol 18: 97-104.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 19735
- [From(publication date):
June-2014 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 14887
- PDF downloads : 4848
