Case Report Open Access
Congenital Cytomegalovirus Infection Diagnosis Case 24 Years Later While Following With The Cerebral Palsy Diagnosis
Yesim Güzey Aras* and Belma Dogan Güngen
Sakarya University Training and Researche Hospital, Turkey
- *Corresponding Author:
- Yesim Güzey Aras
Sakarya University Training and
Researche Hospital, Sakarya, Turkey
Tel: +902642955454
E-mail: yesimguzeyaras@hotmail.com
Received date: July 05, 2017; Accepted date: July 27, 2017; Published date: July 30, 2017
Citation: Aras YG, Güngen BD (2017) Congenital Cytomegalovirus Infection Diagnosis Case 24 Years Later While Following with the Cerebral Palsy Diagnosis. J Neuroinfect Dis 8:257. doi:10.4172/2314-7326.1000257
Copyright: © 2017 Aras YG, et al. This is an open-access article distributed under the terms of the creative commons attribution license, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Cytomegalovirus (CMV) is the most common cause of intrauterine infection, occurring in upto 2% of all live births. Most women are asymptomatic or experience nonspecific symptoms, which can lead to long-term sequelae in newborns including neurological impairment, hearing loss, and mental retardation. In this study, the reveal of congenital CMV diagnosed after the calcification in the brain upon the increasing number of attacks in brain during the treatment with the diagnosis of cerebral palsy, mental retardation and epilepsy is presented.
Keywords
CMV (Cytomegalovirus); Epilepsy; Cerebral palsy
Introduction
Cytomegalovirus (CMV) is a common cause of congenital viral infections. While 90% of all infants with congenital CMV are asymptomatic, 10% of the mare symptomatic [1]. CMV is a highly prevalent infectious agent in the general population, and the rates of the cero positivity in adult women range from between 40% (in most European countries) and 90% (in most African and Asian countries) [2,3]. Congenital CMV infection cases constitute only 5% to 10%, and are asymptomatic in birth with the diagnosis of preterm births i.e., 5-10, intrauterine, microcephaly, chorioretinitis, hepatomegaly, splenomegaly, sensorineural hearing loss, hyperbilirubinemia, retardation in liver functioning tests and petechiae [4]. This study presents a 24-year-old male case diagnosed with congenital CMV infection while following the patient with the case of cerebral palsy, mental retardation and epilepsy diagnosis. Due to the increase in the frequency of attacks, the patient’s Brain CT calcifications and Anti CMV IgG 207 [5-8] were examined.
Case Presentation
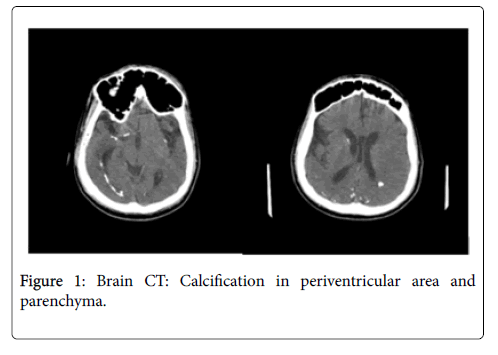
A 24-year-old male was brought to our hospital with the complaint of frequent epileptic seizure. It was learned that the patient was medical history and was born in 2100 g with no infection story of the 30-year-old mother. Starting from the birth, it was also realized that the patient was suffering from microcephaly, epileptic seizure, and retardation of extreme motor and mental growth, not being able to talk and the loss of hearing. It was stated in that the patient was diagnosed with cerebral palsy and antiepileptic treatment. In his systemic examination, there was a microcephalic view with the length of 110 cm and weight of 40 kg. In his neurological examination, he was diagnosed not having the speaking and understanding ability, extreme mental retardation as well as spastic quadriparezi. The patient was given valproic acid with the dose of 600 mg/day for the epileptic seizure. Upon the diagnosis of the increased frequency of the epileptic seizure, Brain CT of the patient was examined, which allowed us to determine the intracranial calcification (Figures 1a and 1b).
After the examination of the serological examinations, Anti CMV IgM 0.15 AU/ml (0.85-1), Anti CMV IgG AU/ml 207 (5.9-6), CMV IgG Avidite AU/ml 75.1 (50-60), Anti rubella IgM 0.14 AU/ml (1.2-1.6), Anti rubella IgG 0.5 AU/ml (5-10) Antitoxoplasma IgM 0.03 AU/ml, Antitoxolpasma IgG 0.3 AU/ml (4.9-10) were diagnosed. These findings led us to diagnose congenital CMV infection.
Discussion
Histologically, mild to moderate cerebrovascular mineralization, predominantly in the basal ganglia, hippocampus, and dentate nucleus, is a common incidental finding in elderly brains and is considered a nonspecific aging phenomenon. There is also a great variety of rare causes of advanced and/or more severe cerebrovascular calcification, mostly in the basal ganglia, such as hypoparathyroidism or pseudohypoparathyroidism (exceptionally hyperparathyroidism), idiopathic cerebrovascular ferrocalcinosis (Fahr disease), hereditary diseases such as Albright’s osteodystrophy, Cockayne’s syndrome, Down’s syndrome, mitochondrial cytopathies (oculocraniosomatic disease, mitochondrial myopathy), birth anoxia, carbon monoxide poisoning, lead intoxication, CNS infection (such as cytomegalic inclusion disease, toxoplasmosis, cysticercosis, herpes or measles encephalitis, and tuberculous meningitis) or hemorrhage, acute leukemia, therapeutic cranial irradiation, and methotrexate therapy [3]. In our case he was diagnosed with congenital cytomegalovirus infection.
Congenital CMV infection is the most common congenital infection worldwide, with an estimated incidence in developed countries that ranges from 0.6% to 0.7% of all live births, resulting in approximately 60,000 neonates born every year with congenital CMV infection in the United States and the European Union combined. Since the incidence of congenital CMV infection parallels maternal seroprevalence, the estimated incidence in developing countries is even higher, between 1 and 5% of all live births [4]. The two known main sources of primary CMV infection during pregnancy are through sexual activity and contact with young children [5]. Infected women often present with nonspecific signs and symptoms, but the majority is asymptomatic. Approximately 10% of new borns show symptoms at birth but this increases to 20% to 30% if their mothers were infected in the first trimester [6]. In this case, the mother was asymptomatic.
There is 30% mortality in the affected infants and 90% will have long-term neurological impairment [7]. The presentation in this latter group is a continuum of disease expression whose more common findings are petechiae, jaundice, hepatomegaly, splenomegaly, microcephaly, and other neurologic signs. Laboratory and imaging findings include thrombocytopenia, transaminitis, and direct hyperbilirubinemia, chorioretinitis, and neuroimaging abnormalities indicative of central nervous system (CNS) involvement [4]. 70% of the congenital CMV infection cases are reported that they may have microcephaly, and that half of these cases may have periventricular calcifications in Brain CT [8]. In our study, it was also diagnosed that there was microcephaly from birth and calcification was observed in periventricular and intraparenchymal regions of the Brain CT. What is more, it is stated that these cases are more associated with mental retardation, hearing loss and chorioretinitis. There was strong mental retardation and the hearing loss in our study as well. However, chorioretinitis was not diagnosed. In their study with 35 patients, Dakovic and etc. observed that 85.7% of the patients had cerebral palsy, 77.1% epilepsy. In our case, there was cerebral palsy and epilepsy.
Conclusion
In conclusion, congenital CMV infection, a disease diagnosed with clinical findings usually revealed in new born period can also be observed in the following ages. This case is presented to emphasize the necessity of getting the cranial image and the importance of keeping the congenital CMV infection in mind with the patients who also suffer from cerebral palsy and epilepsy.
References
- �?�?zdemir �?�?MA, Alkili�?§ L, Yildirim N, Yilmaz E, Adali F (2012) Konjenital sitomegalovir�?¼s infeksiyonu olgu sunumu. Van Tip Dergisi19:189-192.
- Mack I, Burckhardt MA, Heininger U, Pr�?¼fer F, Schulzke S, et al. (2017) Symptomatic congenital cytomegalovirus infection in children of seropositive women. Front Pediatr 5: 134.
- Heron E, Hernigous A, Chatellier G, Fornes P, Emmerich J, et al. (1999) Intracerebral calcification in systemic sclerosis. Stroke30:2183-2185.
- Marsico C, Kimberlin DV (2017) Congenital cytomegalovirus infection: Advances and challenges in diagnosis, prevention and treatment. Marsico and Kimberlin.Ital J Pediatr 43:38.
- Davis NL, King CC, Kourtis AP(2017) Cytomegalovirus infection in pregnancy. Birth Defects Res109:336-346.
- Sullivan CO, Arulkumaran MS, Lakasing L, Jauniaux E, Murphy K (2017) Sequence and timing of intracranial changes in cytomegalovirus in pregnancy: A case report and literature review. Case Reports in Obstetrics and Gynecology Article ID 5928398, 7:5.
- Dogan Y, Yuksel A, Kalelioglu IA, Has R, Tatli B, et al. (2011) Intracranial ultrasound abnormalities and fetal cytomegalovirus infection: Areport of 8 cases and review of the literature. Fetal Diagn Ther 30: 141��?149.
- Baley JE, Toltzis P (2006) Perinatal viral infections. In: Martin RJ, Fanaroff AA, Walsh MC, (eds). Fanaroff and Martin��?s Neonatal-Perinatal medicine diseases of the fetus and infant. Philadelphia, Mosby Elsevier, USA. 840-882.
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 3529
- [From(publication date):
September-2017 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 2718
- PDF downloads : 811