Case Report Open Access
Uncommon Strain for an Intracranial Infection: Bacillus Simplex as Suspected Cause of Brain Abscess
| Alessandro Pesce*, Giada Toccaceli and Giancarlo D Andrea | |
| Neurosurgery Division, NESMOS Department, Sapienza University, Roma, Italy | |
| *Corresponding Author : | Alessandro Pesce Neurosurgery Division, NESMOS Department Sapienza University, Roma, Italy Tel: 393408094246 E-mail: ale_pesce83@yahoo.it |
| Rec date: Jan 21, 2016; Acc date: Mar 17, 2016; Pub date: Mar 19, 2016 | |
| Citation: Pesce A, Toccaceli G, Andrea GD (2016) Uncommon Strain for an Intracranial Infection: Bacillus Simplex as Suspected Cause of Brain Abscess. J Neuroinfect Dis 7:209. doi:10.4172/2314-7326.1000209 | |
| Copyright: © 2016 Pesce A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Brain abscess is a serious life threatening condition. Leading causes include open head injury, history of neurosurgical procedure, dissemination from distant abscessual foci, sepsis, continuity spreading. Most common pathogens involved in genesis of brain abscesses are Streptococcus and Staphylococcus spp. depending on the pathogenetic mechanism. The aim of this study is to report a brain abscess sustained by Bacillus Simplex, a microorganism thought to be responsible of food-borne diseases, whose marginal role is recognized in human pathology, but in this case, for the first time in literature, described as suspected as cause of brain abscess.
| Keywords |
| Brain abscess; Stereotactic evacuation; Cerebral infections; Intraoperative MRI; Antibiotic therapy |
| Introduction |
| Brain abscess is a serious life threatening condition, usually fatal if left untreated [1,2]. Despite rapid progress in the optimization of the antibiotic therapy and the definition of BA incision as gold standard in surgical treatment of BA [3], the death rate caused by such disease is still between 10% in developed countries and 32% in the developing countries [1,3,4]. The factors of intracranial dissemination of BA traditionally described are: infection caused by penetrating cranial trauma and/or neurosurgical procedure; hematologic dissemination by distant abscessual focuses; dissemination by contiguity with proximal abscessual focuses as otitis, sinusitis, periodontal pathology and dental abscesses [1-12]. The aim of this study is to report a brain abscess presumably caused by Bacillus Simplex, a bacteria playing a minor role in human pathology and commonly considered merely responsible for food-borne diseases, here described for the first time in literature as possible cause of brain abscess. |
| Case Report |
| A 51 years old man showing no relevant diseases except arterial hypertension, arrived, in May 2015, at Emergency Room of our institute due to an acute onset right hemiparesis and temporospatial disorientation which gradually improved with intravenous antiedemigenous therapy. |
| A brain CT scan highlighted an hypointense, round formation, with regular margins, in left frontoparietal area. Therefore the patient was admitted at Neurosurgery Unit of our institute. The patient was apyretic. Laboratory findings showed 9500/mm3 WBC (71% Neutrophils, 18.4% Lymphocytes), VES 4 mm/h, CRP (C Reactive Protein) 6.39 mg/dL, Procalcitonin 0.45 ng/dL. The blood and urine cultures were negative. Except for the high levels of CSF proteins and slightly elevated cell count, the lumbar puncture was in a normal range. |
| Total body CT scan ruled out the presence of neoplastic lesions or other abscess foci but showed a vast cavity in right lung apex opening in the right superior lobe bronchus, as for a previous tubercular infection. Cultures from Broncho-Alveolar Lavage and direct Ziehl- Neelsen staining excluded the presence of Koch bacilli or other bacterial strains. Quantiferon test ruled out a latent TB infection. An echocardiogram and X-Ray dental panoramic scan also excluded respectively bacterial endocarditis or odontogenic infections. No evidences of HIV or other immunodepressive condition were observed at laboratory tests. |
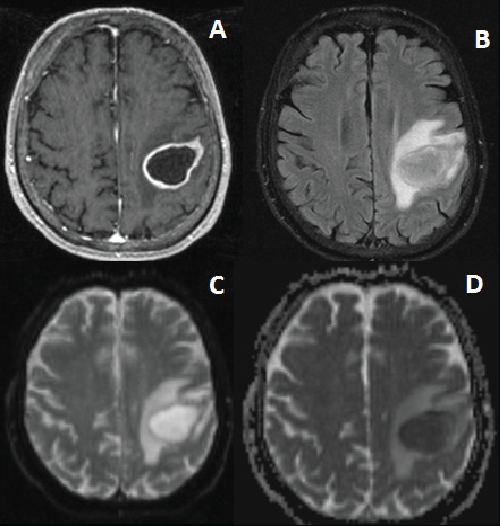
| A T1w, T2w, PWI, DWI and Gadolinium enhanced brain MRI scan was performed and confirmed the presence of a round lesion with a thin and uniform hyperintense periferic ring in Gadolinium enhanced sequences, and by restricted signal in DWI with diameter of 33 mm 48 mm, located in the frontoparietal white matter right below the rolandic and postrolandic cortical areas (Figure 1). |
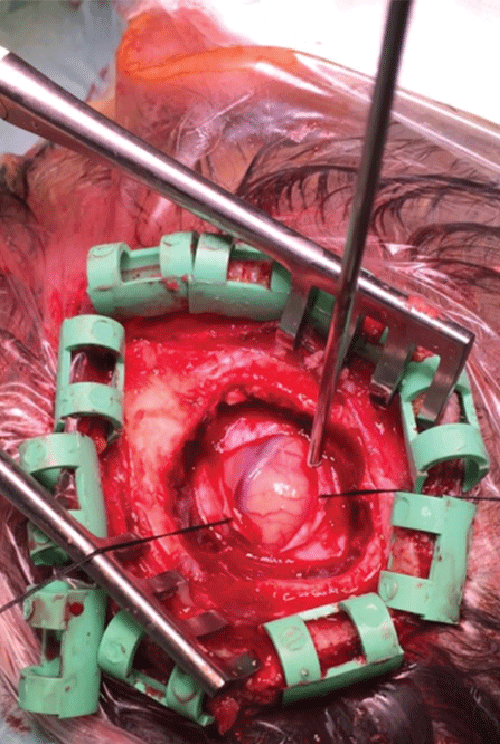
| A conservative strategy with a wide range antibiotic therapy with intravenous Vancomycin 2 gr per day, intravenous Meropenem 2 gr three times per day and after 15 days a brain MRI scan was repeated and confirmed the same findings without relevant modifications of the lesion. Right hemiparesis improved but did not resolve; for the proven drug resistance, for the dimensions greater than 2.5 cm, for the localization in the eloquent cortex and the persistence of the motor disturbances, the patient was operated on with a minimally invasive approach which consisted in mini craniotomy (1.5 cm 1.5 cm), stereotactic incision and evacuation of brain abscess (Figure 2). The purulent content of the cyst was sent to routine microbiologic cultures and then repeated two times for the surprising results: cultures returned a Bacillus Simplex, an extremely uncommon strain in human infectious diseases, for the first time described as responsible of brain abscesses. |
| A postoperative antibiotic therapy with Meropenem 2 gr three times per day was mantained for 30 days. On seventh postoperative day blood examination showed no blood count abnormalities and a dramatic CRP and Procalcitonin improvement (down to 2.9 mg/dL and 0.085 ng/dL respectively). A 20 postoperative days brain MRI scan ruled out the presence of recurrent or residual brain abscess (Figure 3). The preoperative motor deficit gradually recovered in 30-40 days, and patient could turn back to his common daily activities and employment. |
| Discussion |
| The Bacillus Simplex is a strain of Bacillus bacteria that presents a variable gram reaction; two “biovar” of B. Simplex, denominated Biovar 1 and Biovar 2, which differentiate by sugar fermentation, have been classificated. |
| In stressful environmental conditions, bacterial cells produce oval endospores which can remain quiet for long periods. These spores are highly resistant to heat, cold, desiccation, radiation, and disinfectants, and enable the B. Simplex to resist in otherwise inhospitable environments, reactivating in favorable conditions producing vegetative cells. Most strains are strictly aerobic. |
| These Bacteria are generally present in soil, but bacterial strains have been isolated from bread ingredients and bread (13) and, in one case, Genome Sequence of Bacillus simplex has been isolated from a human fecal sample (19). |
| Differently from Bacillus coereus , evident human patogenous activities have not been found; however a potential patogenous activity of the bacterium, related with the presence of thermoresistant toxins pre and post bread cooking, has been object of study. |
| Furthermore in a 2004 study Taylor et al. Have analyzed the capability of B. Simplex and other species of Bacillus of producing a toxin with physical features similar to those of the B. cereus emetic toxin: the cereulide [13-15]. |
| In this study we present a case of brain abscess in which a strain of B. Simplex was isolated. |
| To the best of our knowledge this is the first case of B. Simplex infection and, in particular, brain abscess reported in literature. The specific pathogenic mechanisms for the invasion of the brain tissue have not been previously described and they are not clear, but they have lead, in our case, to the genesis of a suppurative process that caused an early cerebritis, and after to a friable full-formed capsule at the moment of the operation, in which there was a purulent material. |
| Knowledge of the pathophysiology of the abscess capsule as a defense of the host toward the suppurative process, implies that pealing the capsule away is not necessary [16]. Furthermore this manoeuvre has proven to increase morbidity and mortality [17]. Surgical incision of the capsule and evacuation of the suppurative content is the current treatment of choice. The stereotactic technique can lead to a safe and effective minimally invasive craniotomy for evacuation with minimal damage to healthy brain [18,19]. This procedure, recognized as typically mini-invasive (short operative time, negligible blood loss) is feasible even in patients with declined overall medical conditions. A further advantage is to provide a microbial sensitivity test leading to a tailored antibiotic therapy, minimizing therefore the adverse effects of an empirical wide range antibiotic therapy and minimizing selection phenomena of the bacterial strains involved in the abscess. |
| The course of our patient was frankly benign: the patient’s recovery was complete. |
| In spite of the considerable editorial and scientific efforts already made concerning both the experimental phase and the clinical management of serious CNS infections, we believe that there is a lack of a solid base of support and continuous collaboration between clinical and laboratory disciplines experts (Neurosurgeons, Infectious diseases specialists and Clinical microbiologists), to outline and explain, in cases similar to the one reported, every possible virulence factor and pathogenetic mechanism underlying such an uncommon finding. |
References
- Su TM, Lan CM, Tsai YD, Lee TC, Lu CH, et al. (2003) Multiloculated pyogenic brain abscesses: Experience of 25 patients. Neurosurgery 52: 1075-1080.
- Stapleton SR, Bell BA, Uttley D (1993) Stereotactic aspiration of brain abscesses: is this the treatment of choice? Acta Neurochir 121:15-19.
- Carpenter J, Stapleton S, Holliman R (2007) Retrospective analysis of 49 cases of brain abscess and review of the literature. Eur J Clin Microbiol Infect Dis 26:1-11.
- Hakan T, Ceran N, Erdem I, Berkman MZ, Goktas¸ P (2006) Bacterial brain abscess: an evaluation of 96 cases. J Infect 52:359-366.
- Frati A, Pichierri A, Bastianello S, Raco A, Santoro A, et al. (2011) Frameless Stereotactic Cerebral Biopsy: Our Experience in 296 Cases StereotactFunct Neurosurg 89:234-245.
- Broggi M, Broggi G (2015) Stereotactic biopsy: an established procedure, but still modern?, World Neurosurg 83:285-287.
- Leuthardt EC, Wippold FJ, Oswood MC, Rich KM (2002) Diffusion weighted MR imaging in the preoperative assessment of brain abscesses. Surg Neurol 58:395-402.
- Chang SC, Lai PH, Chen WL, Weng HH, Ho JT, et al. (2002) Diffusion-weighted MRI features of brain abscess and cystic or necrotic brain tumors Comparison with conventional MRI. Clin Imaging26:227-236.
- Arlotti M, Grossi P, Pea F, Tomei G, Vullo V, et al. (2010) Consensus document on controversial issues for the treatment of infections of the central nervous system: bacterial brain abscesses. Int J Infect Dis4:79-92.
- Landriel F, Ajler P, Hem S, Bendersky D, Goldschmidt E, et al. (2012) Supratentorial and infratentorial brain abscesses: surgical treatment, complications and outcomes--a 10-year single-center study. Acta Neurochir (Wien)154:903-911.
- Lu CH, Chang WN, Lui CC (2006) Strategies for the management of bacterial brain abscess. J Clin Neurosci13:979-985.
- Kondziolka D, Duma CM, Lunsford LD (1994) Factors that enhance the likelihood of successful stereotactic treatment of brain abscesses. Acta Neurochir (Wien) 127:85-90.
- De Bellis P, Minervini F, Di Biase M, Valerio F, Lavermicocca P, et al. (2015) Toxigenic potential and heat survival of spore-forming bacteria isolated from bread and ingredients. Int J Food Microbiol 197:30-39.
- Taylor JM, Sutherland AD, Aidoo KE, Logan NA (2005) Heat-stable toxin production by strains of Bacillus cereus, Bacillus firmus, Bacillus megaterium, Bacillus simplex and Bacillus licheniformis. FEMS Microbiol Lett 242:313-317.
- Khayi S, Essarts YRD, Mondy S, Moumni M, Helias V, et al.(2015) Draft Genome Sequences of the Three Pectobacterium-Antagonistic Bacteria Pseudomonas brassicacearum PP1-210F and PA1G7 and Bacillus simplex BA2H3. Genome Announc3: e01497.
- Garnett JA, Simpson P, Taylor J, Benjamin SV, Tagliaferri C, et al. (2012) Structural insight into the role of Streptococcus parasanguinis Fap1 within oral biofilm formationBiochemical and Biophysical Research Communications 417: 421-426.
- Liang X, Chen YYM, Ruiz T, Wu H (2011)New Cell Surface Protein Involved in Biofilm Formation by Streptococcus parasanguinisinfection and immunity 79: 3239-3248.
- Chen Q,Sun B, Wu H, Peng Z, Fives-Taylor PM (2007) Differential Roles of Individual Domains in Selection of Secretion Route of a Streptococcus parasanguinis Serine-Rich Adhesin, Fap1. J Bacteriol 189: 7610-7617.
- Croce O, Hugon P, Lagier JC, Bibi F, Robert C,et al. (2014) Genome Sequence of Bacillus simplex Strain P558, Isolated from a Human Fecal Sample. Genome Announc2:e01241-14
Figures at a glance
 |
 |
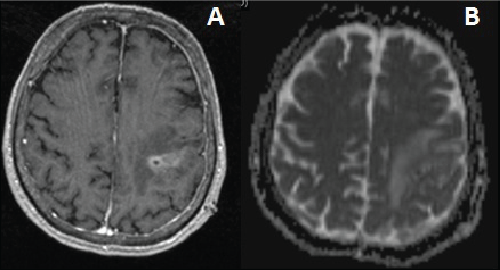 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 13632
- [From(publication date):
March-2016 - Jun 14, 2025] - Breakdown by view type
- HTML page views : 12576
- PDF downloads : 1056
