Research Article Open Access
Transcranial Magnetic Stimulation Therapy in Spastic Cerebral Palsy Children Improves Motor Activity
Meena Gupta1, Bablu Lal Rajak1, Dinesh Bhatia1* and Arun Mukherjee2
1Department of Biomedical Engineering, North Eastern Hill University, Meghalaya, India
2UDAAN-for the differently abled, Lajpat Nagar, New Delhi, India
- *Corresponding Author:
- Dinesh Bhatia
Department of Biomedical Engineering
North Eastern Hill University
Shillong-793022, Meghalaya, India
Tel: +913642723853
E-mail: bhatiadinesh@rediffmail.com
Received Date: October 04, 2016; Accepted Date: November 03, 2016; Published Date: November 05, 2016
Citation: Gupta M, Rajak BL, Bhatia D, Mukherjee A (2016) Transcranial Magnetic Stimulation Therapy in Spastic Cerebral Palsy Children Improves Motor Activity. J Neuroinfect Dis 7:231. doi: 10.4172/2314-7326.1000231
Copyright: © 2016 Gupta M, et al. This is an open-access article distributed under the terms of the creative commons attribution license, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Transcranial magnetic stimulation (TMS) is a new interventional tool used in the study of neuronal activity and treatment of psychiatric disorders. Repetitive TMS (rTMS) is a non-invasive technique of stimulating the brain employing magnetic pulses. Recent research has demonstrated the efficacy of rTMS in facilitating motor functions. Using these evidences, we studied the effectiveness of rTMS in improving motor activity in spastic cerebral palsy (CP) children. CP is a neuro-developmental disorder of movement and posture that is caused by injury to the developing brain that restrict activities of daily living. In the quest to treat CP, several interventions are used among which physical therapy is the mainstay therapy. In this study, we selected 45 spastic CP children and divided them randomly into three groups-the reference group (RG) that was provided only physical therapy (PT) for 30 minutes daily for 20 days; the interventional group (IG) that was administered rTMS frequency of 5Hz (IG-A) and 10Hz (IG-B) for 15 minutes (1500 pulses) daily followed by PT as in RG. Gross motor function measure (GMFM) was used as assessment tool to evaluate the motor performance. Prior to start of therapy, pre-assessment of GMFM was performed on all participants and post assessment after completion of 20 sessions. The result was statistically significant in all three groups (p<0.001) and the mean change demonstrated 0.64%, 1.75% and 2.59% improvement in motor activity among participants in RG, IG-A and IG-B respectively. The study demonstrated positive effect of rTMS in improving motor activity when combined with PT.
Keywords
Cerebral palsy; Gross motor function measure; Physical therapy; Transcranial magnetic stimulation
Introduction
Transcranial magnetic stimulation (TMS) is a unique investigational tool used to study various neural processes and treat a variety of neurological illnesses due to its ability to directly modulate corticospinal and intracortical motor cortex [1]. Repetitive TMS (rTMS) is a non-invasive brain stimulation technique through which a focused magnetic field is delivered by a coil deep into the brain tissue. The repetitive pulses of the magnetic field stimulate neuronal activity in the target brain area by changing the pre-stimulus dynamics of neuronal firing in the stimulated region [2]. Recent studies have established that brain stimulation using rTMS can stimulate motor neurons that facilitate motor function in animals [3,4] and humans [5]. Kirton demonstrated the use of TMS on stroke and cerebral palsy (CP) patients that facilitated motor function after stimulating their motor cortex [6]. He further added that TMS can be employed in CP to study the activity and coordination of different parts of the brain by single or paired (repetitive) TMS pulses and to improve brain function [7].
CP belongs to a group of neurodevelopmental disorder(s) related to motor and posture impairment that develops in early childhood and persists throughout lifespan of an individual [8]. CP is caused by various etiological factors including prematurity, injury to developing brain, perinatal stroke, hypoxia, neonatal inflammation or infections; besides genetic variability [9]. Now-a-days, CP is regarded as a heterogeneous condition with multiple-causes, clinical types, neuropathology patterns, associated developmental pathologies (cognitive impairment, epilepsy, etc.) and rare genetic variations [10]. This heterogeneity gives rise to different forms of CP (spastic, ataxic, dyskinetic, athetoid), among which spastic CP is quite common and found in 70% to 80% of the cases. It is a neuromuscular impairment that limits the movement and posture of the body due to increase in the tonic stretch reflex or exaggerated tendon reflex in the muscles [11]. These patients are not able to perform activities of daily living (ADL) that involve movement and coordination of arm, leg and other body parts and thus fail to achieve developmental activities such as rolling, crawling, sitting, standing and walking. In order to improve the motor performance of spastic CP patients, various interventions [12] are combined with physical therapy such that motor function may be enhanced. Physical therapy (PT) teaches day-to-day movement skills such as sitting, walking, playing and dressing using cast’s orthotics and provides muscle strengthening exercises [13]. In this study, we present our brief finding that demonstrates the effectiveness of rTMS when combined with PT in improving motor functions in spastic CP children in limited number of sessions.
Method
In this study, neuro-MS/D variant-2 therapeutic (Neurosoft, Russia) with angulated coil in the figure of eight (AFEC-02-100-C) and two channels of Neuro-EMG–MS digital system (for determining the motor threshold) were employed. The eight-shaped coil generates a magnetic field of up to 4 Tesla at the center of the coil that easily penetrates the cranium and enters the soft tissue of the brain. In this study, the coil was placed on the primary motor cortex which is known to be the motor pathway. This study was conducted after approval from the institutional ethics committee for human samples or participants (IECHSP), of the host institution and written consent from the parents or guardians of spastic CP children that met our inclusion criteria. Inclusion criteria followed were-willingness to participate; age group between 2 to 15 years; muscle tightness mild to moderate and cognitive deficiency nil to moderate, no metallic implants, no uncontrolled seizures or congenital diseases. Total forty-five children were selected from the out-patient department of UDAAN-for the different abled, Delhi, a non-profit organization that pioneered the rehabilitation of CP children using various interventions. The recruited children were randomly assigned into three groups in equal numbers– reference/ control group (RG), interventional group A (IG-A) and interventional group B (IG-B). RG consisted of 12 participants (mean age: 7.49 SD 4.95; male: 7, female: 5), IG-A consisted of 15 participants (mean age: 7.93 SD 4.86; male: 9, female: 6) and IG-B consisted of 14 participants (mean age: 8.06 SD 4.10; male: 10, female: 4 ). Three participants from RG and one from IG-B did not continue the study due to some unknown reasons; thus, their baseline data was not used for any statistical analysis.
The assessment of gross motor function of recruited children were performed using gross motor function measure (GMFM) which is an internationally approved scale used by trained physiotherapists to monitor motor development in spastic CP patients [14] and for assessing efficacy of any treatment [15]. GMFM is a performance based measure that reflects developmental milestones of a growing child (rolling, crawling, sitting, standing, walking/running) referred to as gross motor abilities of CP patients [16]. GMFM has total 88 assessment items which are grouped into five domains, namely A-lying and rolling (17 items), B-sitting (20 items), C-crawling and kneeling (14 items), D-standing (13 items), and E-walking, running and jumping (24 items). Additionally, GMFCS for CP is a level based scale that evaluates patient’s self-initiated movements, with emphasis on sitting, moving and walking.
In this study, prior to starting the therapies, GMFM pre-assessment was performed on all participants of different groups namely, RG, IGA and IG-B. Participants of RG were provided only PT for 30 minutes daily for 20 days (5 days per week for 4 weeks) whereas children in IGA was administered rTMS of 5Hz frequency and those in IG-B with 10Hz comprising of 1500 pulses (50 pulses per train with total 30 trains having inter-train delay of 20 seconds) for 15 minutes daily for 20 days. The rTMS session of both the groups were followed by PT of 30 minutes daily as given to RG. After completion of 20 sessions of different therapies (only PT and rTMS+PT) administered to different groups, post-assessment of GMFM was performed. It is to be noted that PT and rTMS sessions were provided by trained professionals and the assessment was done by a trained physiotherapist who was kept blinded to the research protocols used in the study.
Statistical Analysis
The pre and post GMFM mean scores for each of the three groups were analyzed with a paired-sample t-test, to determine whether any significant differences existed. The variance and covariance analyses were also performed. Additionally, mean and median GMFM scores were used to evaluate the percentage of functional gain that was brought about in different groups. All statistical analysis was performed using SPSS 20.0 (Armonk, NY, IBM Corp., USA) and Microsoft Excel 2010. The p-value of less that 0.001 was considered statistically significant.
Results
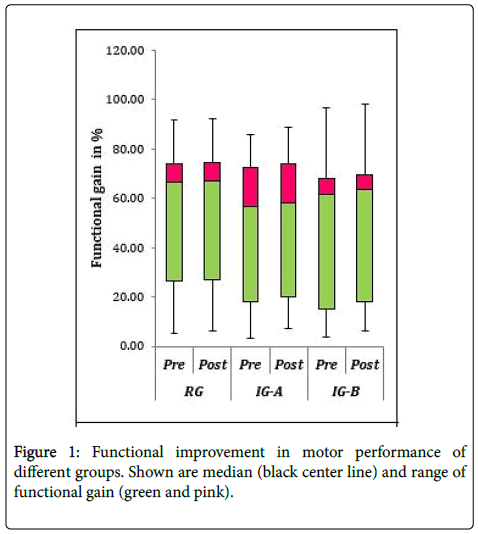
The mean, standard deviation (SD), minimum and maximum GMFM scores of pre and post treatment measures for different groups are given in Table 1. The change between the two measurements for different groups is shown in Figure 1.
| Group | Min | Max | Median | Mean + SD | ||||
|---|---|---|---|---|---|---|---|---|
| Pre | Post | Pre | Post | Pre | Post | Pre | Post | |
| RG | 5.28 | 6.27 | 91.94 | 92.46 | 66.54 | 67.11 | 52.87 + 31.51 | 53.54 + 31.61 |
| IG-A | 3.40 | 7.00 | 86.00 | 88.81 | 56.78 | 58.28 | 48.97 + 29.74 | 50.72 + 29.73 |
| IG-B | 3.53 | 6.27 | 96.94 | 98.46 | 61.45 | 63.59 | 48.57 + 31.37 | 51.17 + 31.01 |
Table 1: Descriptive statistics of reference and interventional groups.
The paired t-test between the pre and post assessment of GMFM scores in reference (only physical therapy) group (RG) revealed significant differences (t=-7.784, df=11, p=0.0001, confidence interval (CI) -0.864 to -0.483). The mean change score was 0.64 (SD 0.29). The paired t-test between pre and post assessment of GMFM scores in interventional (r-TMS +PT) groups were also significant. In IG-A, t= -7.382, df= 14, p<0.0001, CI-2.258 to -1.242 and in IG-B, t= -8.424, df= 13, p<0.0001, CI-3.257 to -1.927. The mean change score was 1.75 (SD 0.92) in IG-A and 2.59 (SD 1.15) in IG-B. Therefore, it can be stated that physical therapy (in RG) and r-TMS followed by PT (in IG-A, IGB) had a significantly positive effect on the gross motor function in spastic CP children.
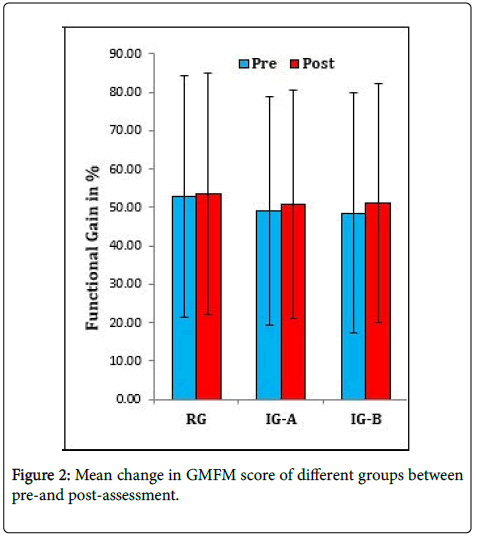
Statistical analysis reveal that the improvement in gross motor function for children of interventional group that was administered rTMS pulses was significantly greater than those in reference group. The result confirmed that rTMS combined with PT could cause greater progress in children’s motor activity. Additionally, from the mean change scores it was observed that 0.64% progress was obtained following only PT in one month but when rTMS pulses was administered prior to PT, the improvement was appreciable i.e., 1.75% and 2.59% with 5Hz and 10Hz frequency respectively in similar time duration (Figure 2). Also, it was noted that 10Hz r-TMS frequency brought greater improvement as compared to 5Hz as evident from the mean change scores of IG-A and IG-B.
Discussion and Conclusion
Our study was based on the previous work done employing rTMS by different research groups hat established the fact, if brain stimulation is given repeatedly it can produce lasting changes in brain function with potential therapeutic effects [17,18]. The high frequency rTMS (above 5 Hz to 10 Hz) stimulates the motor cortex area of the brain which facilitates motor function in animals and humans. Recent studies on spinal cord injury (SCI), multiple sclerosis and stroke patients provide good evidence to show the effectiveness of r-TMS on motor function. Kumru et al. study on improvement of motor score and gait pattern demonstrated that high-frequency rTMS combined with rehabilitation therapy can be more effective in the management of motor impairment and spasticity than rehabilitation therapy alone [19]. A similar finding was reported by Elkholy et al. with improved gait patterns in stroke patients [20]. Moreover, Mally and Dinya reported improvement in paretic extremities with rTMS in stroke patients when the traditional rehabilitation had failed [21]. Following evidences from the reported literatures in improvement of motor functions; we conducted this study in spastic CP children to evaluate their motor development. Our findings in the study demonstrate the effectiveness of rTMS in spastic CP cases. Thus, it can be concluded that the administration of high frequency rTMS prior to PT can lead to significant progress in motor function. The improved motor activity in spastic CP children can be attributed to the significant reduction in muscle tightness of both upper and lower extremities due to the stimulating effects of rTMS [22].
Furthermore, the benefit of rTMS demonstrated in our study, provide encouraging results for those who advocate this approach, but we do not consider that the results of this one study should be interpreted as the final answer to the above important question, given that some of the earlier studies have reported weak responses to the TMS therapy. Our research team is working to further evaluate the effectiveness of rTMS using different parameters for different diseased groups in children and also to establish its consistency over a period of time in maintaining the improvement it has induced.
Nevertheless, since CP is regarded as heterogeneous spectrum disorder represented by different clinical types, co-morbidities, pathways and genetic variants, it is of much concern that despite different etiological factors contributing to CP causation; there has been little change in the prevalence of this disorder (2-3 per 1000 births) around the world [10]. Thus, the recent research paradigm shifts towards the genetic factor being responsible for CP. A study conducted in 2005, with a four-generation family of nine (9) children that suffered congenital CP, found that a 225 kb deletion on chromosome 9p24.3 might be responsible for the initiation of CP [23]. In addition, ankyrin repeat domain 15 (ANKRD15), the only protein coding gene within this region (chromosome 9p24.3), is interpreted as a maternal imprinted gene, since the healthy fathers of the sick child, who harbor the same deletion, expresses the normal level of this gene. However, no correlation was found between the expression of the ANKRD15 and the pattern of DNA methylation. Traditionally, it is known that DNA methyltransferases (DNMTs) play a key role in the maintenance of imprinted DNA methylation [24]. Interestingly, recent observation indicated that some histone modifiers, such as G9a and GLP, are also involved in the maintenance of genomic imprinting [25]. Therefore, aberrantly established H3K9me2, the G9a/GLP-associated heterochromatin mark, might directly cause abnormal expression of ANKRD15 and lead to initiation of CP in humans. Thus, investigation of the levels of G9a and GLP in patients might shed light towards new direction for the treatment of this neurological disorder.
Acknowledgment
This work is supported by funding received (Ref: SEED/TIDE/ 007/2013) from the Technology Intervention for Disabled and Elderly of the Department of Science and Technology (DST), Government of India, New Delhi. The authors also acknowledge the support of all the staffs of UDAAN-for the differently abled, Delhi. The authors are grateful to the children and their parents for participating in this sponsored study.
References
- Valero-Cabre A, Pascual-Leone A (2005) Impact of TMS on the primary motor cortex and associated spinal systems. IEEE Eng Med Biol Mag 24: 29-35.
- Ridding MC, Rothwell JC (2007) Is there a future for therapeutic use of transcranial magnetic stimulation?. Nature Rev Neurosci 8: 559-567.
- Adkins-Muir DL, Jones TA (2003) Cortical electrical stimulation combined with rehabilitative training: enhanced functional recovery and dendritic plasticity following focal cortical ischemia in rats. Neuro res 25: 780-788.
- Plautz EJ, Barbay S, Frost SB, Friel KM, Dancause N, et al. (2003) Post-infarct cortical plasticity and behavioral recovery using concurrent cortical stimulation and rehabilitative training: a feasibility study in primates. Neuro res 25: 801-810.
- Hallett M (2000) Transcranial magnetic stimulation and the human brain. Nature 406: 147-150.
- Kirton, A (2013) Modulation of Developmental Plasticity with Non-Invasive Brain Stimulation in Cerebral Palsy. Int J Phys Med Rehabil 1: 2.
- http://www.neurodevnet.ca/sites/default /files/neurodevnet/download/tms.pdf
- Koman LA, Smith BP, Shilt JS (2004) Cerebral palsy. Lancet 363:1619-1631.
- Lungu C, Hirtz D, Damiano D, Gross P, Mink JW (2016) Report of a workshop on research gaps in the treatment of cerebral palsy. Neurology 87:1293-1298.
- MacLennan AH, Thompson SC, Gecz J (2015) Cerebral Palsy: causes, pathways, and the role of genetic variants. Am J Obstet Gynecol213:779-788.
- Odeen I (1980) Reduction of muscular hypertonus by long-term muscle stretch. Scand J Rehabil Med 13:93-99.
- Sénéchal C, Larivée S, Richard E, Marois P (2007) Hyperbaric oxygenation therapy in the treatment of cerebral palsy: a review and comparison to currently accepted therapies. JAmPhys Surg 12: 109.
- Damiano DL (2006) Activity, activity, activity: rethinking our physical therapy approach to cerebral palsy. Phys Ther 86(11): 1534-1540.
- Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, et al. (1997) Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol 39: 214-223.
- Feng J, Du L, Shan L, Wang B, Li H (2015) Infra-low Frequency Transcranial Magnetic Stimulation Effectively Improves the Motor Function in Children with Spastic Cerebral Palsy. J Neurol Neurophysiol 6:2.
- Russell DJ, Rosenbaum PL, Cadman DT, Gowland C, Hardy S, et al. (1989) The gross motor function measure: a means to evaluate the effects of physical therapy. Dev Med Child Neurol 31: 341-352.
- Pascual-Leone A, Tormos JM, Keenan J, Tarazona F, Cañete C, Catalá MD (1998) Study and modulation of human cortical excitability with transcranial magnetic stimulation. JClin Neurophysiol 15: 333-343.
- Khedr EM, Ahmed MA, Fathy N, Rothwell JC (2005) Therapeutic trial of repetitive transcranial magnetic stimulation after acute ischemic stroke.Neurology 65: 466-468
- Kumru H, Benito J, Murillo N, Valls-Sole J, Valles M, et al. (2013) Effects of high-frequency repetitive transcranial magnetic stimulation on motor and gait improvement in incomplete spinal cord injury patients. Neurorehabil Neural Repair 27: 421-429.
- Elkholy SH, Atteya AA, Hassan WA, Sharaf M, Gohary AME (2014) Low Rate Repetitive Transcranial Magnetic Stimulation (rTMS) and Gait Rehabilitation after Stroke. Int J Neurorehabil 1: 2376-2381.
- Mally J, Dinya E (2008) Recovery of motor disability and spasticity in post-stroke after repetitive transcranial magnetic stimulation (rTMS). Brain Res Bull 76: 388-395.
- Gupta M, Rajak BL, Bhatia D, Mukherjee A (2016) Effect of r-TMS over standard therapy in decreasing muscle tone of spastic cerebral palsy patients. J Med Eng Technol 40: 210-216.
- Lerer I, Sagi M, Meiner V, Cohen T, Zlotogora J, et al. (2005) Deletion of the ANKRD15 gene at 9p24.3 causes parent-of-origin-dependent inheritance of familial cerebral palsy. Hum Mol Gen14:3911-3920.
- Okano M, Bell DW, Haber DA, Li E (1999) DNA methyltransferases Dnmt3a and Dnmt3b are essential for de novo methylation and mammalian development. Cell 99:247-257.
- Zhang T, Termanis A, Özkan B, Bao XX, Culley J, et al. (2016) G9a/GLP complex maintains imprinted DNA methylation in embryonic stem cells. Cell rep 15:77-85.
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 16680
- [From(publication date):
December-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 15541
- PDF downloads : 1139