Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
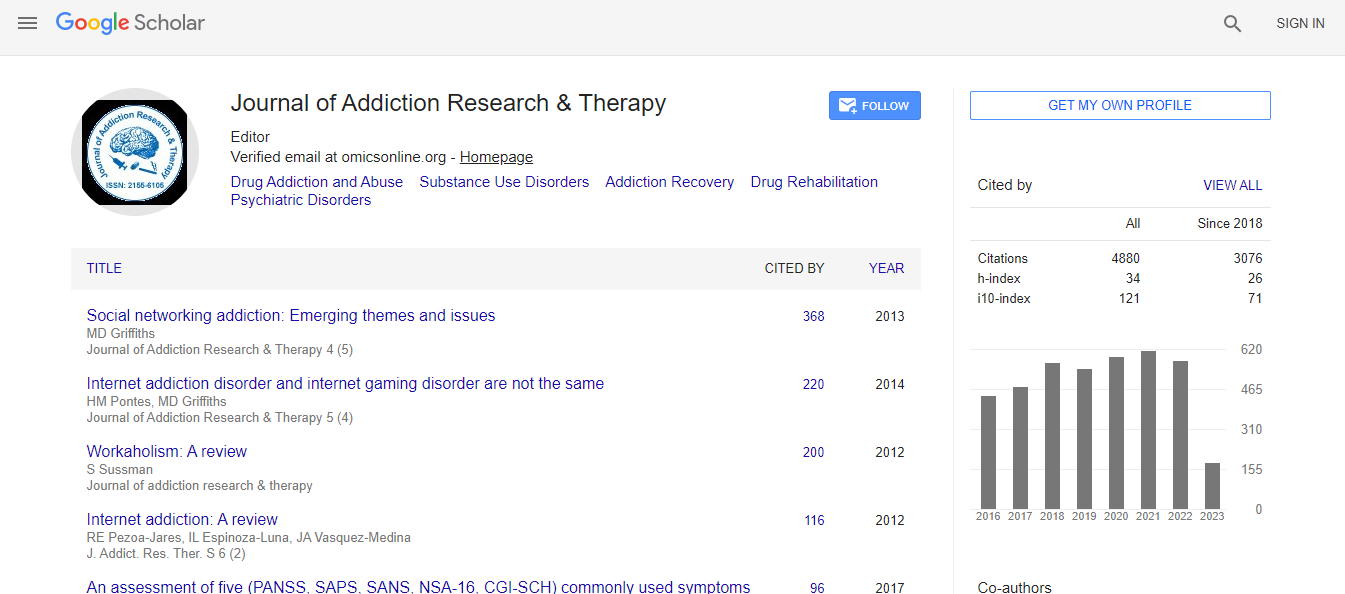
Google Scholar citation report
Citations : 4859
Journal of Addiction Research & Therapy received 4859 citations as per Google Scholar report
Journal of Addiction Research & Therapy peer review process verified at publons
Indexed In
- CAS Source Index (CASSI)
- Index Copernicus
- Google Scholar
- Sherpa Romeo
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- SafetyLit
- China National Knowledge Infrastructure (CNKI)
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- SWB online catalog
- Virtual Library of Biology (vifabio)
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Reward Deficiency Solution System(RDSS): Changing the landscape of treatment and relapse prevention for all addictions utilizing evidence- based research in humans and animal models
2nd International Conference and Exhibition on Addiction Research & Therapy
Kenneth Blum
Keynote: J Addict Res Ther
Abstract
We evaluated the potential association of dopamine D2 receptor gene (DRD2), dopamine D1 receptor gene (DRD1), dopamine transporter gene (DAT1) and dopamine beta-hydroxylase gene (DBH) polymorphisms in Reward Deficiency Syndrome (RDS) subjects derived from two families. We illustrated the relevance of a generalized RDS behavior set as the phenotype. We genotyped an experimental group of 55 subjects derived from up to five generations of two independent multiple-affected families compared to very rigorously screened controls. We found significant association with only the DRD2 A1 allele and DAT1 10 allele and RDS behaviors: 78% carried the DRD2 Taq1 allele, 58% carried the DAT1 10/10 allele, 66% carried the DBHB1 allele and 35% carried either the DRD1 A1/A1 or A2/A2 genotypes. We genotyped 70 patients using a 9 reward gene polymorphic (18 allele) panel including: DRD 2, 3, 4; MOA-A; COMT; DAT1; 5HTTLLR; OPRM1; and GABRA3. Low severity (LS) = 1-36%; Moderate Severity =37-50%, and High severity = 51-100%. Fourteen Percent had low risk whereas, 81% had moderate risk and 5% had high risk.We utilized the Comprehensive Analysis of Reported Drugs [CARD] on 5,703 patients and 11, 403 specimens, to systematically evaluate both compliance and abstinence (risk for relapse) during treatment in various treatment settings across six eastern states.We found compliance to prescribed medications during recovery treatment across six eastern states to be only 67 percent, whereas only 39% of these patients were found to be abstinent from drugs of abuse. 92 % of patients in opioid treatment utilizing methadone were compliant, only 49 % of these patients were abstinent. Suboxone maintenance patients were compliant at 88% but only 48% were abstinent based on CARD. Surprisingly, in the Suboxone and Methadone groups we found high opioid misuse approximately at 47%. Utilizing an accurate voice recognition system we found a flat affect in long-term Suboxone patients. These results indicate the need to incorporate the Reward Deficiency Solution System in treatment and is currently being tested in human and animal modelsBiography
Kenneth Blum is widely designated as Father of Psychiatric Genetics because of the of the DRD2 gene and its correlation with various psychiatric disorders including the Reward Deficiency Syndrome (RDS) which term he has coined. He is also known as the Father of Neuro- Nutrient Therapy for his discovery of successful nutrient therapy for RDS. He holds numerous domestic and foreign patents and is co-founder and Chairman & CSO of LifeGen Inc. He is a former Full Professor in the Department of Pharmacology, University of Texas Health Science Center ,San Antonio, Texas; Volunteer Professor in the Department of Psychiatry & McKnight Brain Institute, University of Florida College of Medicine, Gainesville, Florida and Adjunct Full Professor of Psychiatry at the University of Vermont College of Medicine, Burlington, Vermont. He currently serves as Neuroscience advisor for Dominion Diagnostics., LLC North Kingstown, Rhode island, Malibu Beach Recovery Center, Malibu Beach California, and is the Scientific Director of PATH Foundation NY, New York. He is an honorary Faculty of IIOAB, India. He has been recently appointed Chief Scientific Officer(CSO) of G&G Holistic Addiction Treatment Centers in North Miami Beach Florida. To his credit he has over 400 publications in peer reviewed journals, 14 books and has received many awards including a Lifetime Achievement Award from the National Institute of Holistic Addiction Studies.

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi