Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
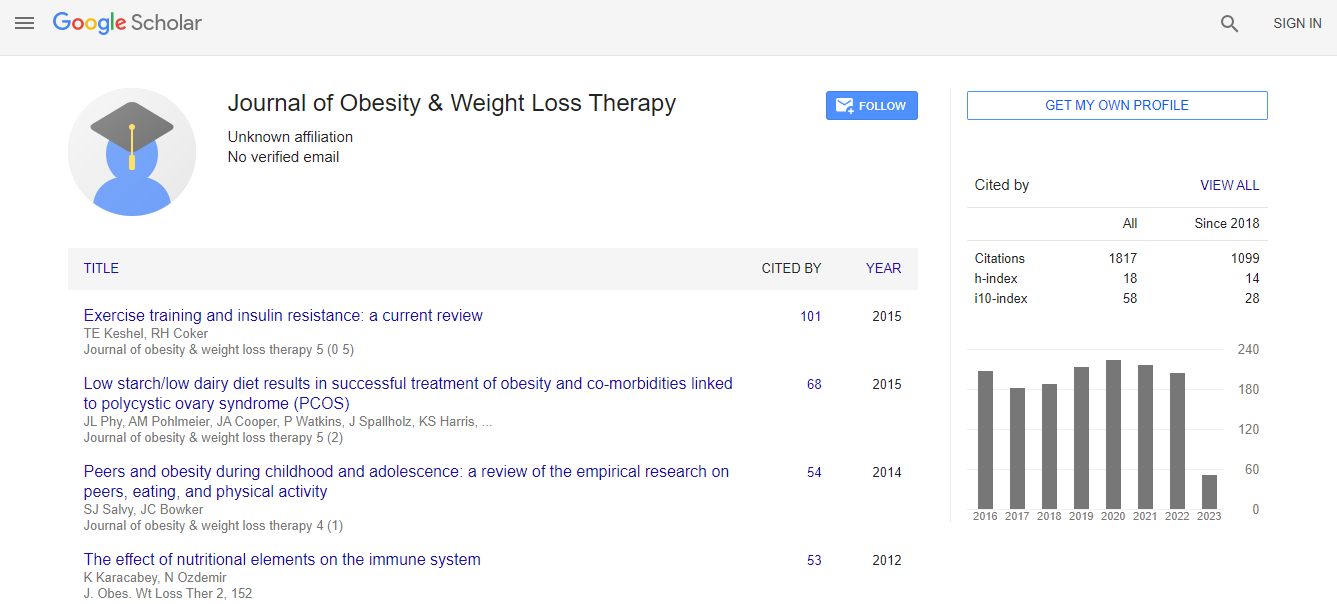
Google Scholar citation report
Citations : 2305
Journal of Obesity & Weight Loss Therapy received 2305 citations as per Google Scholar report
Journal of Obesity & Weight Loss Therapy peer review process verified at publons
Indexed In
- Index Copernicus
- Google Scholar
- Open J Gate
- Genamics JournalSeek
- Centre for Agriculture and Biosciences International (CABI)
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- SWB online catalog
- CABI full text
- Cab direct
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
- University of Bristol
- Pubmed
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Laparoscopic sleeve gastrectomy versus laparoscopic adjustable gastric banding � Perspective from rural Australia
4th International Conference and Exhibition on Obesity and Weight Management
Ya Chu May Tsai1, H M Tsai2, J Muir3, S Clifforth3 and W Ooi4
1St Vincent�s Hospital, Australia 2Monash University, Australia 3Western District Health Service, Australia 4University of Melbourne, Australia
ScientificTracks Abstracts: J Obes Weight Loss Ther
Abstract
Aim/Objective: Obesity affects over 60% of Australian population and bariatric surgery is increasingly used to address this issue. However, there is limited literature in the Australian rural context. Our objective was to compare outcomes of laparoscopic sleeve gastrectomy (LSG) and laparoscopic adjustable gastric banding (LAGB) performed in rural Australia. Methods: Retrospective review of consecutive patients who underwent LAGB and LSG by a single surgeon at a rural hospital in Victoria, Australia were obtained from bariatric database. The main outcomes measured were major complications and weight loss over time, expressed as percentage of excess body weight loss (% EWL) and Body Mass Index loss (BML kg/m2). Results: 140(58.1%) and 101 patients (41.9%) underwent LSG and LAGB respectively. No mortality was recorded. Three patients (2%) returned to theatre due to staple line leak post LSG. Only 1(1%) patient in the LABG required return to theatre for re-adjustment of band. Post op blood transfusion rates were 2% (3patients) and 1% (1patient) in the LSG and LABG group respectively. 7 other patients (5%) undergoing LSG encountered post op complications (6 patients at electasis, 1patient a trial fibrillation) compared to 1 patient in LABG group with pulmonary embolus. LSG group had a higher pre-operative BMI (45.05�±6.84kg/m2) compared to LAGB group being 43.15�±6.73kg/m2 (p<0.05). LSG provided significantly greater (p<0.05) weight loss after 18 months (% EWL 68.75�±13.05% and BML 11.73 �± 6.44 kg/m2) compared to LAGB (% EWL 46.15�±23.85% and BML 8.13�±5.44kg/m2) Conclusions: Bariatric surgery can be performed safely in rural Australia with comparable results to international standards. LSG is more effective than LABG in achieving weight loss.Biography
Ya Chu May Tsai is currently a Doctor at St Vincent’s Hospital Melbourne Australia after completing her MBBS/B Med Science at the University of Melbourne in 2013. She has been involved in cardiovascular medicine research with Professor Andrew Wilson and has published in the International Journal of Cardiology. Her area of interests includes cardiology and peri-operative medicine. She is currently completing Postgraduate Certificate/Diploma in Clinical Ultrasound.
Email: maytsai1990@gmail.com

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi