Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
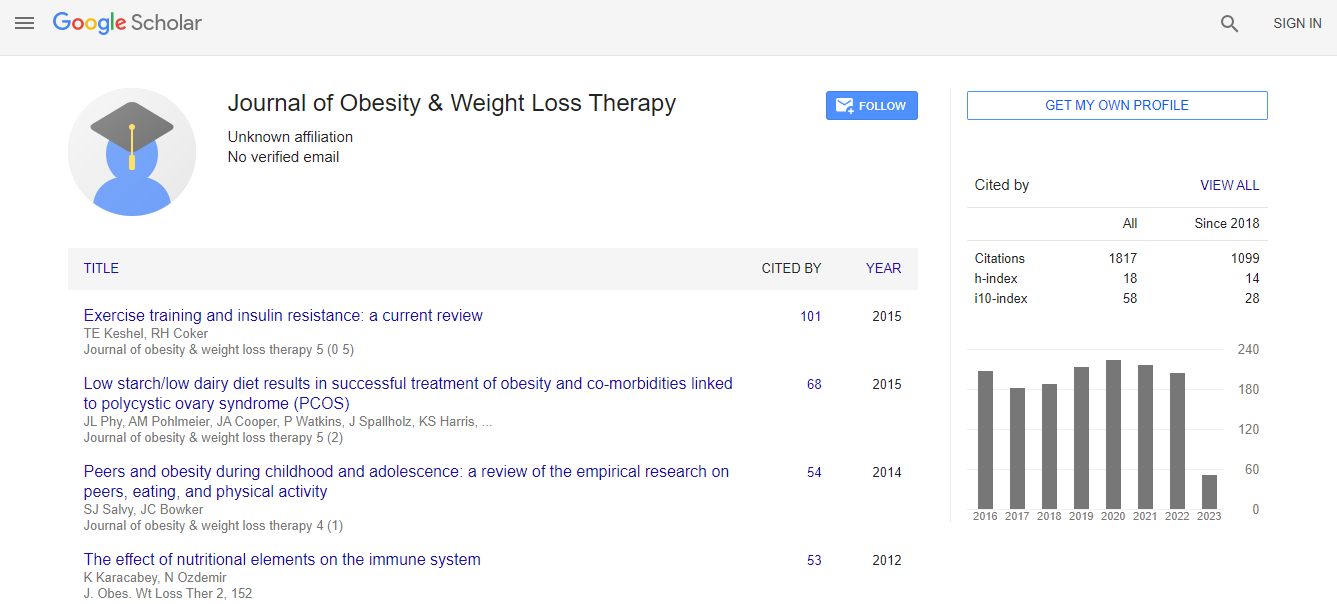
Google Scholar citation report
Citations : 2305
Journal of Obesity & Weight Loss Therapy received 2305 citations as per Google Scholar report
Journal of Obesity & Weight Loss Therapy peer review process verified at publons
Indexed In
- Index Copernicus
- Google Scholar
- Open J Gate
- Genamics JournalSeek
- Centre for Agriculture and Biosciences International (CABI)
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- SWB online catalog
- CABI full text
- Cab direct
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
- University of Bristol
- Pubmed
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Laparoscopic wedge resection of gastrojejunostomy for weight recidivism after gastric bypass
JOINT EVENT 10th International Conference on Childhood Obesity and Nutrition & 2nd International Conference on Metabolic and Bariatric Surgery
Aly Elbahrawy
McGill University Health Centre, Canada
Posters & Accepted Abstracts: J Obes Weight Loss Ther
Abstract
Background & Aim: Weight recidivism after Roux-en-Y gastric bypass (RYGB) is a common problem. Often, this weight loss failure or regain may be due to a wide gastrojejunostomy (GJ). We evaluated the feasibility and safety of a novel approach of laparoscopic wedge resection of gastrojejunostomy (LWGJ) for a wide stoma after RYGB associated with weight recidivism. Methods: This is a single-center retrospective study of a prospectively-collected database. We analyzed outcomes of patients with weight recidivism after RYGB and a documented wide GJ (>2 cm) on imaging, who underwent LWGJ between 11/2013-05/2016. Results: Nine patients underwent LWGJ for dilated stomas. All patients were female with a mean�?±SD age of 53�?±7 years. Mean interval between RYGB and LWGJ was 9�?±3 years. All cases were performed laparoscopically with no conversions. Mean operative time and hospital stay were 86�?±9 minutes and 1.2�?±0.4 days, respectively. The median (IQR) follow-up time was 14 (12-18) months. During follow-up, there were no deaths, postoperative complications or unplanned readmissions or reoperations. The mean and median (IQR) BMI before RYGB and LWGJ were 55.4�?±8.1 kg/m2 and 56.1 (47.9-61.7) and 43.4�?±8.6 kg/m2 and 42.1 (38.3-47.1), respectively. One year after LWGJ, mean and median (IQR) BMI significantly decreased to 34.9�?±7.3 kg/m2 and 33.3 (31.7-35.0) corresponding to a mean %EWL of 64.6�?±19.9 (P<0.05). Conclusion: LWGJ is safe and can lead to further weight loss in patients experiencing weight recidivism after RYGB with a wide GJ (>2 cm). Long-term follow-up is needed to determine the efficacy and durability of LWGJ and compare its outcomes with other endoscopic/surgical approaches for weight recidivism after RYGB with a documented wide GJ.Biography
Email: aly.elbahrawy@mail.mcgill.ca

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi